Phenotypic Sex Differentiation
Unlike the bipotential gonads and
external genitalia, the male and female internal genitalia arise from separate
duct systems (Fig. 6.1). Development of these structures occurs in parallel and
in close physical proximity with the developing urinary system. Both begin to
occur at about 4 embryonic (6 menstrual) weeks. The primordial kidney
(mesonephros) is composed of tubules and a duct known as the mes- onephric or
Wolffian duct. The Wolffian duct grows out from the tubules toward the
urogenital sinus. The mesonephric tubules make contact with the primitive sex
cords just as the gonad begins to differentiate. Simultaneously, an inpocketing
of the coelomic epithelium near the lateral edge of the mesonephric ridge forms
the paramesonephric or Müllerian duct. As kidney development proceeds
(metanephric stage), the mesonephric structures will become totally
incorporated into the reproductive tract and lose their urinary function. The
Wolffian and Müllerian ducts are primordia for the internal organs of
reproduction in the male and female, respectively. In each sex, the other duct
system typically disappears by the 3rd fetal month, leaving behind vestiges
that are usually unimportant clinically.
In the normal male embryo, the
secretion of a peptide called Müllerian-inhibiting substance (MIS; also known
as anti-Mullerian hormone or AMH) occurs
under the direction of sex-determining region of the Y chromosome (SRY). MIS is
secreted by cells that will become Sertoli cells in the adult testis. MIS
causes the Müllerian duct to degenerate. Testosterone is produced by those
testicular cells des- tined to become Leydig cells in the adult. Testosterone
directs development of the Wolffian duct system to form the epididymis,
vas deferens and seminal vesicles. In contrast to the adult,
testosterone production by the embryonic testes is controlled not by the
hypothalamic-pituitary system, but by the placental hormone human chorionic
gonadotropin (hCG).
The absence of MIS in the female
embryo permits the Müllerian system to persist. Upon reaching the urogenital
sinus, the Müllerian ducts induce the formation of a vaginal plate. Contact of
the Müllerian ducts with the vaginal plate also initiates the fusion of the
ducts to form the body of the uterus. The Müllerian ducts will form the fallopian
tubes, uterus and the upper portion of the vagina. Failure of
the Müllerian ducts to develop or fuse completely can cause uterine and
cervical anomalies. In the absence of testosterone, the Wolffian system
regresses. A vestige of the Wolffian duct, known as Gartner’s duct, persists in
its length from the ovary to the hymen. Clinically apparent cysts may form
anywhere along Gartner’s duct.
Most
of the prostate gland develops from the same primordial area of the
urogenital sinus that forms the vaginal plate in the female, making the
prostate a homolog of the upper vagina. Mesenchyme in this tissue
differentiates into the peripheral zone of the prostate, under the influence of
dihydrotestosterone (DHT). In the presence of a functional fetal testis,
DHT is produced locally from testosterone by the enzyme 5α-reductase. The more
central tissue in this area, which may be of Wolffian derivation, forms the
central and transition zones of the prostate. Cancers of the prostate are most
likely to arise from the peripheral zone (Chapter 41).
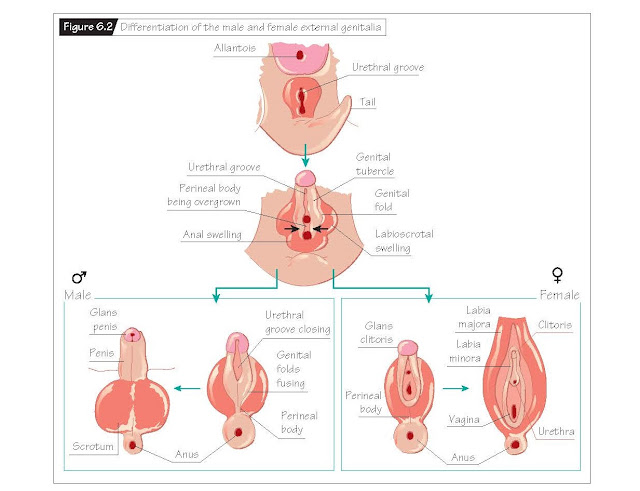
External genitalia
Like the primordial gonads, the
anlagen of the external genitalia are bipotential. In the 8th embryonic (10th
menstrual) week, a urogenital slit, a genital tubercle, two lateral genital
folds and two labioscrotal swellings become apparent as precursors to the
external genitalia (Fig. 6.2).
While differentiation of the
internal Wolffian duct system is testosterone dependent, the primordial
external genital structures require the presence of DHT to differentiate into
recognizably male structures. The source of the DHT is testicular testosterone,
converted locally to DHT in the primordial external genitalia. In the presence
of DHT, the lobes of the prostate gland grow out from the seminal colliculus
where the urethra is developing from the bladder. The genital folds fuse to
form the penis around the elongating urethra. The labioscrotal swellings
enlarge and fuse to form the scrotum.
Descent of the testes from the
abdomen into the scrotum is an androgen-dependent event during which the testes
are pulled down- ward by a fibrous cord anchored to the developing scrotum –
the gubernaculum. During development, a peritoneal fold around the Wolffian
and Müllerian ducts (destined to eventually become the tunica vaginalis) connects to the genital
swelling, and the gubernaculum forms as a ridge under the peritoneum. The
gubernaculum connecting the testis to the genital swelling does not grow as rapidly
as the remainder of the embryo and hence each testis is progressively pulled
down toward the developing scrotum. The testes sit just above the inguinal ring
until the last 3 months of pregnancy, at which time they complete their descent
through the inguinal canal into the scrotum. After full descent of the testes,
the inguinal canal narrows, thereby preventing abdominal contents from
herniating into the scrotum. Unlike differentiation of the external and
internal genitalia that relies on placental hCG stimulation of testicular
androgen production, testicular descent requires fetal gonadotropins.
Disruptions in the fetal hypothalamic–pituitary–testicular axis result in
failure of the testes to descend properly (cryptorchidism).
In the female, the folds of the
urogenital slit remain open. The posterior aspect of the urogenital sinus forms
the lower two-thirds of the vagina and the anterior aspect forms the
urethra. The lateral genital folds form the labia minora and the
labioscrotal swellings form the labia majora. The clitoris forms
above the urethra. The gubernaculum that forms between the edge of the
Müllerian duct and the ovary becomes secondarily attached to the cornua of the
uterus as it differentiates. The gubernaculum in the female becomes the ovarian
and round ligaments. Female phenotypic differentiation occurs in the absence of
androgen and is not dependent on an ovary.
Exposure to specific androgens
beginning in the 5th embryonic (7th menstrual) week of pregnancy is critical to
the development of a recognizable newborn male phenotype. Fetuses exposed to
endogenous or exogenous DHT at this time will undergo male differentiation,
regardless of the genetic or gonadal sex. Lack of androgen activity will result in a female phenotype.



.webp)

