KAPOSI’S SARCOMA
Kaposi’s
sarcoma is a rare malignancy of endothelial cells seen in unique settings. The
classic variant is seen in older patients, most commonly individuals living in
the region surrounding the Mediterranean Sea. Kaposi’s sarcoma associated with
human immunodeficiency virus (HIV) infection or with acquired immunodeficiency
syndrome (AIDS) is seen predominantly in men, and the tumor is thought to be
caused by human herpesvirus-8 (HHV8). There is also a variant seen in
chronically immunosuppressed patients, such as those who have undergone solid
organ transplantation. The African cutaneous variant of Kaposi’s sarcoma is
seen in younger men in their third or fourth decade of life. Kaposi’s sarcoma
is a locally aggressive tumor that rarely has a fatal outcome. The one
exception is the very rare African lymphadenopathic form of Kaposi’s sarcoma,
which is distinct from the more common African cutaneous form.
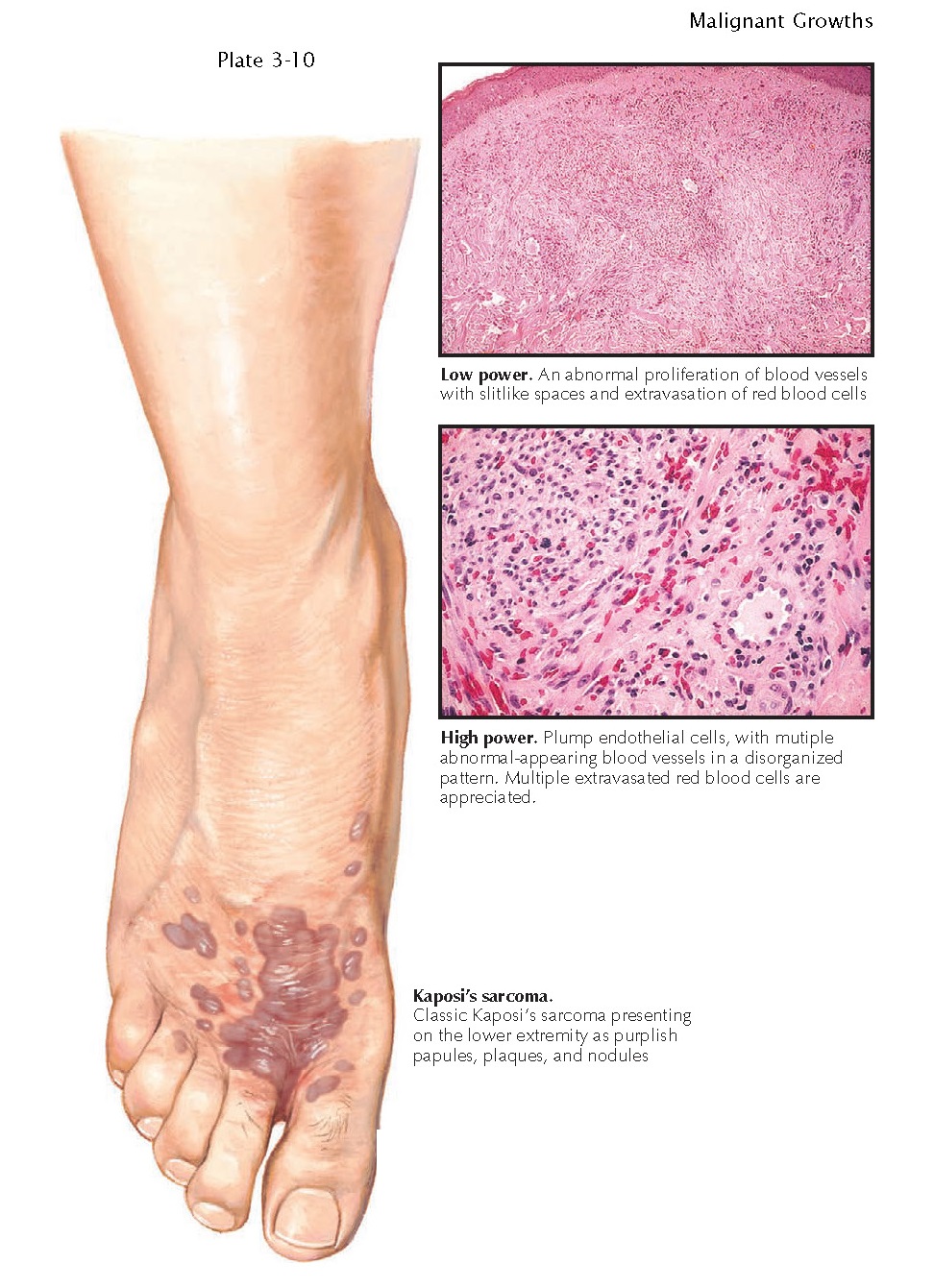
Clinical Findings: The tumors are very similar in appearance across
the subtypes of clinical settings. They usually appear as pink-red to purple
macules, papules, plaques, or nodules. In the classic form of Kaposi’s sarcoma,
the tumors are most often found on the lower extremities of older men. Some tumors
in this setting remain unchanged for years, and the patient often dies of other
causes. Occasionally, the tumors grow and ulcerate, causing pain and bleeding.
The disseminated form of classic Kaposi’s sarcoma can be very aggressive, and
patients require systemic chemotherapy.
AIDS-associated Kaposi’s sarcoma is
the most common form of the disease. It is most often seen in younger men. In
comparison with the classic form, this form usually manifests as purple
macules, plaques, and nodules on the head and neck, trunk, and upper
extremities. This is an AIDS-defining illness. Patients with AIDS-associated
Kaposi’s sarcoma are at a higher risk for internal organ involvement. The small
bowel has been reported to be the internal organ most commonly affected by Kaposi’s
sarcoma, but it can affect any organ system. Since the advent of multiple-drug
therapy for HIV infection, the incidence of AIDS-associated Kaposi’s sarcoma
has decreased dramatically.
Tropical African cutaneous Kaposi’s
sarcoma is most often seen in younger men. The clinical findings are not much
different from those of the classic form of Kaposi’s sarcoma. These patients
are much more likely to suffer from severe lower-extremity edema. The tumor
also has a higher incidence of bone invasion than the other types. The main
difference between the classic and the African forms of Kaposi’s sarcoma is the
age at onset. The aggressive form of African Kaposi’s sarcoma occurs in
childhood and is often fatal because of its aggressive ability to metastasize.
The lymph nodes are often involved before the skin is. The reason the African
forms act so differently from each other is poorly understood.
Pathogenesis: The pathogenesis of the classic and African forms
of Kaposi’s sarcoma is unknown. The cell of origin of this tumor is believed to
be the endothelial cell. Matrix metalloproteinases 2 and 9 have been shown to
increase angiogenesis and increase the tissue invasion of the affected
endothelial cells. Kaposi’s sarcoma associated with AIDS or other immunosuppressive
states is believed to be caused by the action of HHV8 in a genetically
predisposed individual. HHV8 is thought to cause dysregulation of the immune
response in the afflicted endothelial cells, allowing them to proliferate
uncontrolled by normal immune functions.
Histology: Biopsies of Kaposi’s sarcoma show many
characteristic findings. The promontory sign is often seen; it is represented
by plump endothelial cells jutting into the lumen of the capillary vessel. Many
slit-like spaces are also seen. These spaces represent poorly formed blood
vessels, which are thin walled and easily compressed. They are filled with red
blood cells. The tumor in general is very vascular, with a predominance of
vascular spaces and a large amount of red blood cell extravasation into the
dermis.
Treatment: For classic Kaposi’s sarcoma, the mainstay of
therapy has been localized radiation treatment. Many other treatments have been
advocated, including topical alitretinoin, imiquimod, intralesional vincristine,
and interferon. Systemic chemotherapy for disseminated and aggressive forms is
indicated and is usually based on a regimen of either vinblastine, paclitaxel,
bleomycin, or pegylated liposomal doxorubicin.