SECRETION AND
ACTION OF VASOPRESSIN
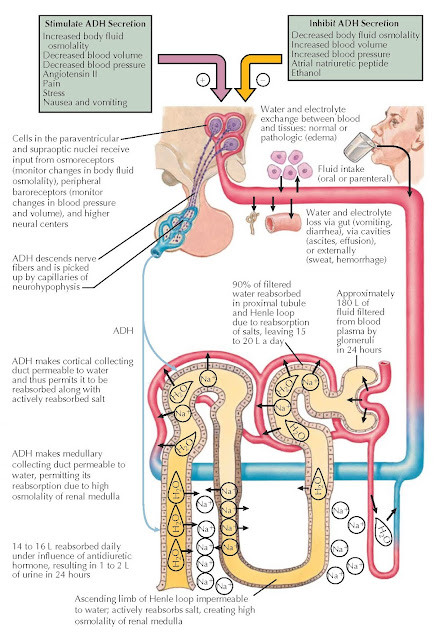
Vasopressin, also known as antidiuretic hormone (ADH), is the key hormone involved in the regulation of water homeostasis and osmolality of body fluids. The secretion and action of vasopressin are regulated by osmotic and pressure/volume factors. Osmoreceptors continuously monitor plasma osmolality. The osmoreceptors are outside the blood–brain barrier, are located in the organum vasculosum of the lamina terminalis (adjacent to the anterior hypothalamus near the anterior wall of the third ventricle), and are perfused by fenestrated capillaries. The normal extracellular fluid osmolality determined to a major degree by serum sodium concentration varies from 282 to 287 mOsm/ kg in healthy individuals. The keys to maintaining this narrow normal range are (1) the very sensitive osmore-ceptor-regulated response of vasopressin secretion to changes in plasma osmolality, (2) the prompt response of urine osmolality to changes in plasma vasopressin, and (3) the short plasma half-life of vasopressin (~15 minutes). Thus, small increases in plasma osmolality result in a prompt increase in urine concentration, and small decreases in osmolality result in prompt water diuresis.
 |
| Plate 1-26 |
Over 24 hours, glomerular filtration
presents 180 L of isoosmotic fluid to the proximal convoluted renal tubules.
Ninety percent of the filtered water is reabsorbed in the proximal tubule
without the help of vasopressin. This passive transfer of water is determined
by the active reabsorption of solutes (e.g., sodium and chloride) taking along
water by osmotic forces. Thus, proximal tubular urine remains isoosmotic with
plasma. Distal collecting duct reabsorption of water is control- led by
vasopressin. The loop of Henle and the collecting duct in the kidney are
critical to water conservation. The countercurrent multiplier system in the
loop of Henle generates a high osmolality in the renal medulla. The ascending,
or distal, limb of Henle loop actively transports sodium without water from the
tubular urine to the interstitial fluid of the renal medulla, making it very
hypertonic. The water impermeability of this limb of Henle loop renders the
urine entering the distal tubule hypotonic with respect to plasma. In the
absence of vasopressin, the distal tubule and collecting ducts remain largely
impermeable to water, and very dilute urine leaves the kidney. With maximum
vasopressin secretion, urine osmolality plateaus at approximately 1000 to 1200
mOsm/kg, limited by the maximal osmolality of the inner renal medulla. When
vasopressin is absent, 14 to 16 L of urine is excreted per day.
The site of action of vasopressin is
the V2 receptor on the epithelial principal cells of the collecting ducts.
Activation of the collecting duct V2 receptor increases water permeability to
allow for osmotic equilibration between the urine and the hypertonic medullary
interstitium. Thus, water is extracted from the urine into the medullary
interstitial blood vessels, causing an increased urine concentration and
decreased urine volume. Aquaporins are intracellular organelles, or water
channels, that mediate rapid water transport across collecting duct cell
membranes. V2-receptor activation by vasopressin increases intracellular cyclic
adenosine monophosphate (cAMP) levels by activating adenylate cyclase. cAMP
activates protein kinase A, which phosphorylates aquaporin-2 and induces a
fusion of aquaporin-2–containing intracytoplasmic vesicles with the apical
plasma membranes of the principal cells, thus increasing
apical water permeability by markedly increasing the number of water-conducting
pores in the apical plasma membrane. The aquaporin-containing vesicles are
shuttled into and out of the membrane in response to changes in intracellular
cAMP levels, resulting in a minute-to-minute regulation of renal water
excretion in response to changes in circulating vasopressin.
Water intake is also a key factor in
maintaining water homeostasis. Increases in plasma osmolality of the extracellular fluid or decreases in intravascular
volume stimulate thirst. Thirst is regulated by osmoreceptors in the anterior
hypothalamus and baroreceptors in the chest. The sensation of thirst is
typically triggered by a 2% increase in plasma osmolality. Because of
unregulated fluid ingestion (e.g., coffee, tea, soft drinks, and water from
metabolized food), thirst does not represent a major regulatory mechanism and,
in a typical healthy person, excess water is excreted daily by the
osmoregulated secretion of vasopressin.


.webp)

