Diverticula of Small
Intestine
A diverticulum is a blind
outpouching of a hollow viscus, consisting of one or more layers of the part
involved. Small intestinal diverticula usually occur in the duodenum and occur
less frequently in the jejunum and ileum. The true incidence is not known,
because diverticula may remain asymptomatic and the diagnosis is usually
incidental; duodenal diverticula have been reported in 7% of those undergoing
endoscopic retrograde cholangiopancreatography. In about 20% of cases, they are
associated with diverticula in other parts of the digestive tract.
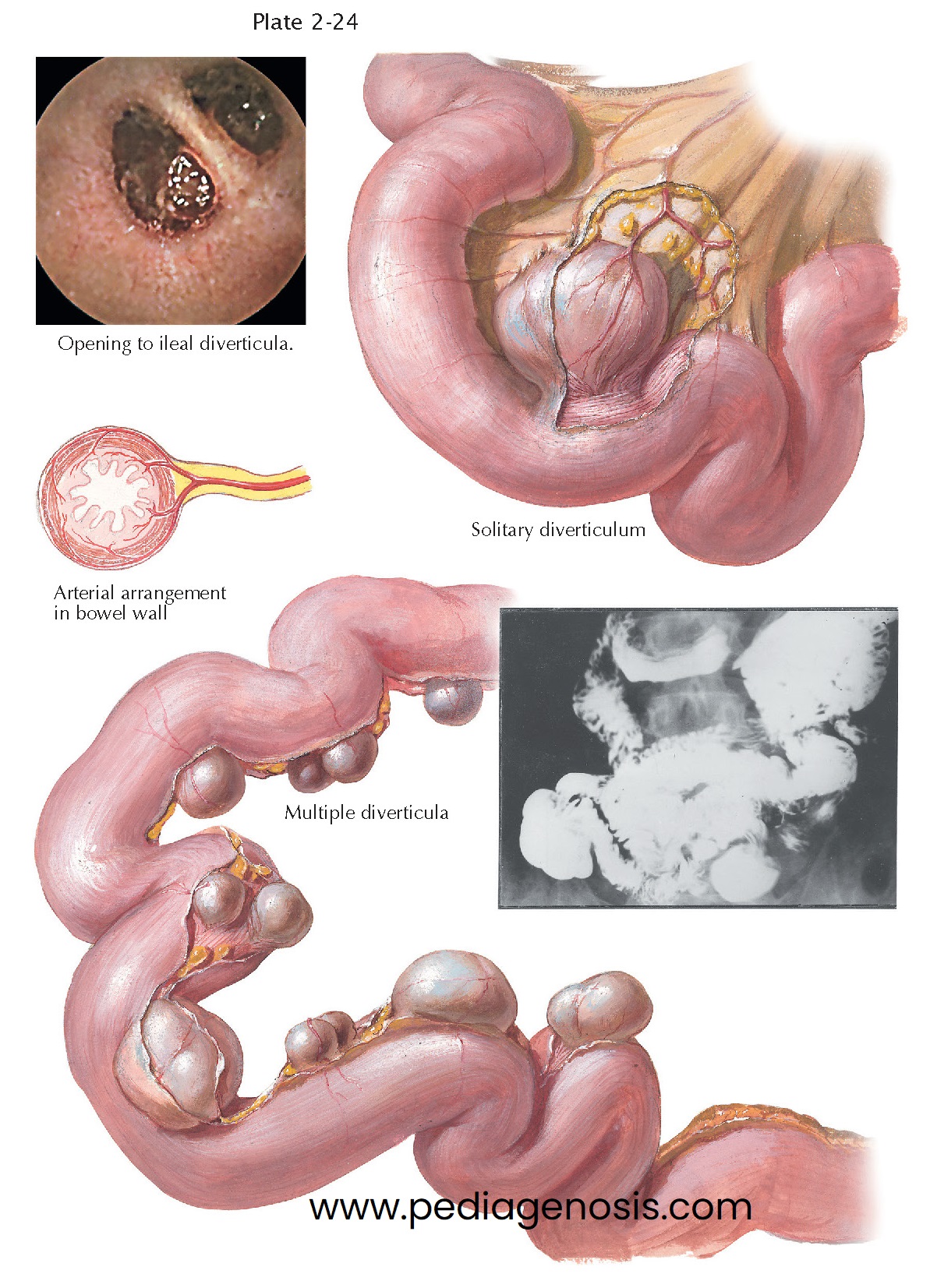
Diverticula of the small intestine may be single or multiple. Jejunal diverticula are usually multiple and are frequently associated with disorders of intestinal motility, such as progressive systemic sclerosis, visceral neuropathies, and myopathies. The multiple diverticula can be so numerous as to involve nearly the entire small intestine. They are located almost always along the line of mesenteric attachment, with sizes varying from a few millimeters up to several centimeters in diameter. The “complete” diverticula, formed by all the layers of the intestinal wall, are believed to be of congenital origin and are frequently associated with other malformations. The “incomplete” diverticula, consisting only of mucosa and serosa, are caused by herniation through a defect caused by the entrance of large vessels.
Diverticula of the small intestine are frequently symptomless and are found incidentally on imaging or endoscopy or at autopsy. In some cases, the symptoms are limited to a vague abdominal pain and flatulence appearing a certain time after meals and attributed to retention of fecal matter in the diverticula. Small intestinal diverticula may, however, give rise to serious complications, such as acute inflammation, intestinal obstruction, perforation, and hemorrhage. Acute diverticulitis is usually the consequence of food residue or parasites becoming trapped in the pouch and may present with symptoms similar to those of acute appendicitis. Intestinal obstruction may occur by strangulation, compression by an inflammatory tumor, or, more rarely, intussusception. Perforation of a diverticulum is usually the consequence of acute inflammation or trauma produced by a foreign body that found its way into the pouch. The perforation may occur in the free abdominal cavity, the mesentery, or another intestinal loop, resulting in generalized peritonitis, a walled-off abscess, or an intestinal fistula. A few cases are recorded in which aberrant pancreatic tissue and benign or malignant tumors were located in an intestinal diverticulum. The presence of massive diverticulosis of the small intestine may lead to bacterial overgrowth, which can seriously interfere with absorption, causing steatorrhea, megaloblastic anemia, and other symptoms that characterize the malabsorption syndrome (see Plate 2-29). Diverticula of the small intestine can be diagnosed only by endoscopic imaging or x-ray studies. X-ray demonstration is, however, rendered difficult when the wide neck of the diverticulum makes it empty readily or when the intestinal contents fill the diverticulum and prevent the entrance of the barium. In patients with asymptomatic diverticula, no treatment is required; management of acute diverticulitis and diverticular bleeding is similar to that for colonic diverticular disease. Small intestinal bacterial overgrowth can be treated with oral antibiotics, but this is rarely curative unless the underlying risk factor (diverticulosis) is removed, and patients require intermittent antibiotic therapy.


.webp)

