Thoracic Wall Anatomy
The skin covering the thorax receives
its nerve supply from lower cervical and upper thoracic spinal nerves. Above
the level of the manubriosternal joint, C4 gives cutaneous innervation, while
tho- racic nerves T2–T11 provide the dermatomes for the remainder of the
thoracic wall. The first thoracic nerve does not contribute to the cutaneous
nerve supply of the thorax but innervates some of the skin of the upper limb
(Figs 1.35 & 3.6).
The breast (Fig. 2.8) consists of glandular tissue and a quantity of
fat embedded in the subcutaneous tissue of the anterior chest wall. In the male
and immature female, the gland is rudimentary. Although the size and shape of
the breast in the adult female vary, the base (the part lying on the deep
fascia covering pectoralis major, serratus anterior
and rectus abdominis) is constant in posi- tion. In the adult female, the base
is roughly circular and extends between the second and sixth ribs. Medially,
the gland overlies the lateral border of the sternum. Part of the breast
extends upwards and laterally and reaches the anterior fold of the axilla.
This is the axillary tail (process)
and is the only part of the breast to penetrate beneath the deep fascia. During
clinical palpation of the breast it is essential that the axillary tail is
included as part of the physical examination.
The glandular elements consist of
15–20 lobes arranged radially, each draining into a lactiferous duct. These
ducts open independently onto the surface of the nipple. The nipple is
surrounded by an area of pink skin, the areola, which may develop brown
pigmentation during pregnancy.
The gland is traversed by fibrous
septa (ligaments of Astley Cooper) (Fig. 2.8), which subdivide the lobes and loosely attach
the skin of the breast to the deep fascia covering the chest wall. In certain
types of breast carcinoma, these fibrous septa may produce characteristic
dimpling of the skin over the lesion. Normally, the breast is freely mobile
over the underlying muscles. However, lack of mobility when pectoralis major is
contracted indicates that breast pathology has fixed the gland to the
underlying chest wall muscles.
Blood supply
The fat and glandular elements of the
breast receive blood from arteries that also supply the deeper structures of
the chest wall. These vessels include perforating branches from the internal
tho- racic artery (internal mammary artery) and the second, third and fourth
intercostal arteries. The lateral thoracic and thoracoacromial arteries arising
from the axillary artery also supply the breast. The gland is drained by veins
that accompany the arteries.
Lymph drainage
Within the substance of the breast,
the lymphatic vessels form a system of interconnecting channels that collect
lymph from all parts of the organ. The superior and lateral aspects of the
breast usually drain into central and apical axillary nodes via infraclavicular
and pectoral nodes. It is therefore important to palpate axillary lymph nodes
in suspected cases of malignant breast disease. The medial and inferior parts
of the breast drain deeply into glands along the internal thoracic vessels and
thence via the bronchomediastinal lymph trunk into the confluence of lymphatic vessels
in the root of the neck (p. 330). Lymphatics may also cross the midline to
communicate with vessels in the opposite breast.
The outer surfaces of the ribs, costal
cartilages and sternum give attachment to muscles involved in movements of the
upper limb and the scapula, namely pectoralis major, pectoralis minor and
serratus anterior. In addition, the external surfaces of the lower ribs provide
attachment for rectus abdominis and the external
oblique muscles of the anterior abdominal wall (pp 143, 144).
This large fan-shaped muscle (Fig.
2.9) attaches to the
clavicle, sternum and upper costal cartilages and forms the bulk of the
anterior wall of the axilla. The clavicular head is attached to the anterior
surface of the medial half of the clavicle. The sternocostal head is anchored
to the manubrium and body of the sternum, and to the upper six costal
cartilages. Laterally, both parts of the muscle attach to the humerus along the
lateral lip of the intertubercular sulcus (p. 77).
Pectoralis major is supplied by the
medial and lateral pectoral nerves from the brachial plexus. Functionally, it
is a powerful adductor and flexor of the arm at the shoulder joint and also
produces medial rotation of the humerus. When the upper limb is fixed, the
sternocostal part may act as an accessory muscle of inspiration by elevating
the ribs.
Pectoralis minor
This small muscle (Fig.
2.10) lies deep to
pectoralis major and is usually attached to the third, fourth and fifth ribs.
The muscle converges on the medial border of the coracoid process of the
scapula. Pectoralis minor is supplied by the medial and lateral pectoral nerves
and assists in movements of protraction and rotation of the scapula.
This large muscle lies between the
scapula and chest wall and attaches to the
lateral aspects of the upper eight ribs (Fig. 2.11), forming part of the medial wall of the axilla.
The muscle fibres from the upper four ribs attach to the superior angle and to
the costal surface of the medial border of the scapula. The fibres from ribs
5–8 converge on the costal surface of the inferior angle of the scapula.
Innervation is provided by the long
thoracic nerve arising in the neck from the upper three roots (C5, C6 & C7)
of the brachial plexus. The muscle is a powerful protractor of the scapula and
assists trapezius in producing scapular rotation during abduction of the upper
limb. In addition, the muscle helps to stabilize the scapula during movements
of the upper limb.
Intercostal spaces
The interval between two adjacent ribs
is called an intercostal space. On each side of the thorax there are 11 such
spaces, numbered from above and occupied by muscles, membranes, nerves and vessels.
The number given to each intercostal space and its neurovascular structures
corresponds to that of the rib which limits the space superiorly. The nerves
and vessels immediately inferior to the twelfth ribs are termed the subcostal
nerves and vessels. The intercostal nerves and vessels supply the intercostal muscles
and the parietal pleura deep to each space. Branches from these vessels also
supply the overlying muscles of the body wall, the superficial fascia and skin.
Most intercostal nerves have cutaneous branches that supply the skin covering
the chest and abdominal walls.
There are three layers of intercostal
muscles, which lie superficial, intermediate and deep. These are named the
external, the internal and the innermost intercostal muscles.
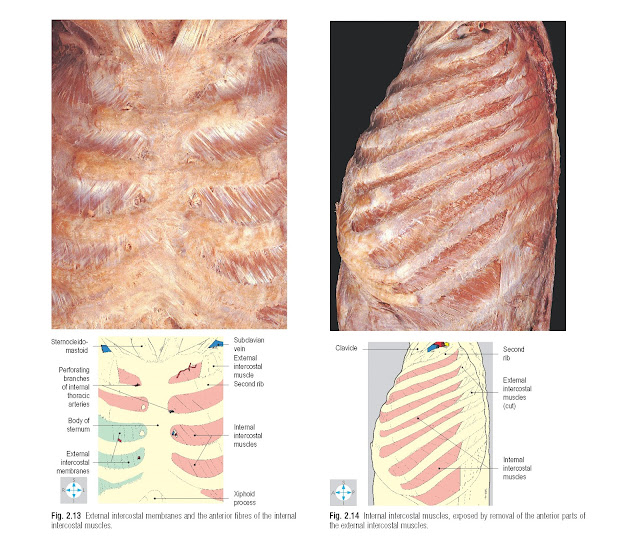
The fibres of the external intercostal
muscles slope downwards and forwards from the lower border of one rib to the
upper border of the subjacent rib (Fig. 2.12). The muscle extends from the
tuber- cle of the rib posteriorly to the junction of the rib and its costal
cartilage anteriorly. Between costal cartilages the muscle fibres are replaced
by a thin fascial sheet, the external intercostal membrane, which reaches the
lateral border of the sternum (Fig. 2.13).
Internal intercostal muscles
The internal intercostal muscles (Fig.
2.14) lie immediately deep
to the external intercostal muscles. The fibres of the two muscles are mutually
at right angles, those of the internal intercostal muscles running downwards
and backwards from the lower border of one rib to the upper border of the
subjacent rib. Ante- riorly, each muscle continues between the costal
cartilages to reach the lateral border of the sternum (Fig. 2.13). Posteriorly, each muscle extends only to the
angles of the ribs, where it is replaced by the internal intercostal membrane,
which continues as far as the tubercles of the ribs.
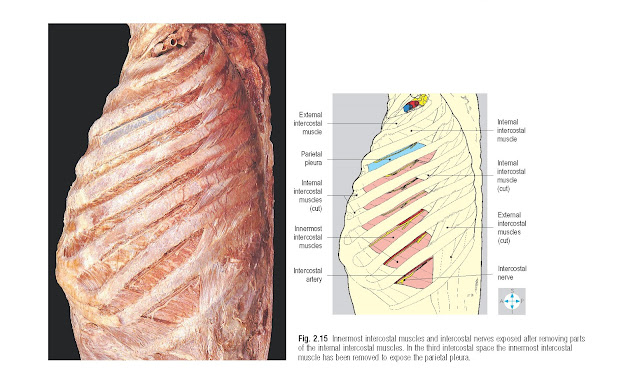
These muscles lie on a plane deep to
that of the internal intercostal muscles (Fig. 2.15). They form the lateral part of an incomplete
layer of muscle which includes the transversus thoracis (sterno- costalis) anteriorly (Fig. 2.16) and
subcostalis posteriorly. The innermost intercostal muscles connect the inner
surface of each rib to that of its neighbours.
All the intercostal muscles in a
particular intercostal space are supplied by the corresponding intercostal
nerve.
Although the main role of the
intercostal muscles is in ventilation of the lungs, it must be emphasized that
during normal, quiet breathing, the muscles of the thoracic wall make only a
small contribution. Inspiration is usually
brought about mainly by the diaphragm, whose descent increases the vertical
diameter of the thorax. The transverse and anteroposterior diameters of the
thorax are increased, especially in deep inspiration, by the external
intercostal muscles, which incline the ribs outwards, upwards and forwards, so
that the intercostal spaces are widened. During quiet breathing, expiration is
largely due to the ‘elastic’ recoil of the
lungs and thoracic wall and involves
minimal activity by the intercostal muscles. Even when expiration is ‘forced’,
for example during vigorous physical exertion or when coughing, the main
muscular effort is provided by the muscles of the abdominal wall rather than
the chest wall. However, the internal intercostal muscles contribute to forced
expiration by drawing the ribs down-wards and inwards, thereby narrowing the
intercostal spaces.
Intercostal vessels and nerves
Each intercostal space has a principal
artery, vein and nerve, which collectively form the neurovascular bundle (Fig.
2.15). This bundle lies in
the neurovascular plane between the internal and innermost intercostal muscles
and runs along the upper part of the intercostal space, occupying the costal
groove of the rib. Usually, the vein lies superiorly and the nerve inferiorly
in the bundle. A collateral nerve and collateral vessels arise posteriorly from
the neurovascular bundle and run forwards along the lower border of the
intercostal space to supply the intercostal muscles.
Intercostal arteries
Intercostal arteries enter from both anterior
and posterior ends of the intercostal space. Anteriorly, the internal thoracic
arteries (internal mammary arteries) (Fig. 2.16) arising from the subclavian
arteries in the root of the neck (p. 330) provide branches that run laterally
to supply the upper six pairs of intercostal spaces. On each side, the lower
five spaces receive anterior intercostal arteries from the musculophrenic
artery, one of the terminal branches of the internal thoracic artery. These
anterior arteries anastomose end-to-end with the posterior intercostal
arteries.
Posterior intercostal arteries to the
lower nine intercostal spaces arise as direct branches from the descending
thoracic aorta (Fig. 2.64). For the first and second spaces, the posterior intercostal
arteries are derived from the intercostal branch of the costocervical trunk.
This trunk arises from the subclavian artery (p. 331) and its intercostal
branch enters the thorax by crossing the neck of the
first rib. The anastomoses between anterior and posterior intercostal
arteries in the lower nine intercostal spaces and between the scapular arteries
and posterior intercostals are important because they enable blood to reach the
descending aorta when the aortic arch is abnormally narrowed (coarctation of
the aorta).
Anteriorly, the intercostal veins from
the lower five intercostal spaces drain into the musculophrenic veins. The
upper six intercostal veins and the musculophrenic veins drain into the
internal thoracic veins, which themselves are tributaries of the
brachiocephalic veins in the root of the neck. Posteriorly, the intercostal
veins drain into the azygos venous system. On the right, those in the lower
eight spaces terminate directly in the azygos vein (Fig. 2.64). The veins from
the second and third spaces combine into a single vessel, the right superior
intercostal vein, which drains into the arch of the azygos vein. The first
posterior intercostal vein (supreme intercostal vein) leaves the thorax to
terminate in the root of the neck, usually in the right vertebral vein.
On the left, the lower eight posterior
intercostal veins enter either the hemiazygos or accessory hemiazygos veins
(Fig. 2.65).
The left superior intercostal vein
drains the second and third spaces and crosses the left side of the arch of the
aorta to terminate in the left brachiocephalic vein (Fig. 2.57). As on the
right the first posterior intercostal vein (supreme intercostal vein) leaves
the thorax to terminate usually in the vertebral, but occasionally in the
brachiocephalic, vein.
Intercostal nerves
The intercostal nerves comprise the
anterior rami of the upper 11 thoracic spinal nerves. Each intercostal nerve
enters the neurovascular plane posteriorly (Fig. 2.65) and gives a collateral
branch that supplies the intercostal muscles of the space. Except for the
first, each intercostal nerve gives off a lateral cutaneous branch near the
midaxillary line, which pierces the overlying muscle (Fig. 1.36). This
cutaneous nerve divides into anterior and posterior branches, which supply the
adjacent skin. The intercostal nerves of the second to the sixth spaces enter
the superficial fascia near the lateral border of the sternum and divide into
medial and lateral cutaneous branches.
Most of the fibres of the anterior
ramus of the first thoracic spinal nerve join the brachial plexus for
distribution to the upper limb (p. 80). The small first intercostal nerve is
the collateral branch and supplies only the muscles of the intercostal space,
not the overlying skin.
The intercostal nerves of the lower
five spaces continue in the neurovascular plane beyond the costal margin to
supply the muscles and skin of the abdominal wall (p. 145).






.webp)

