Erection and Erectile Dysfunction
Penile
erection is essentially a neurovascular event. Upon sexual stimulation, nerve
impulses release neurotransmitters from the cavernous nerve terminals and
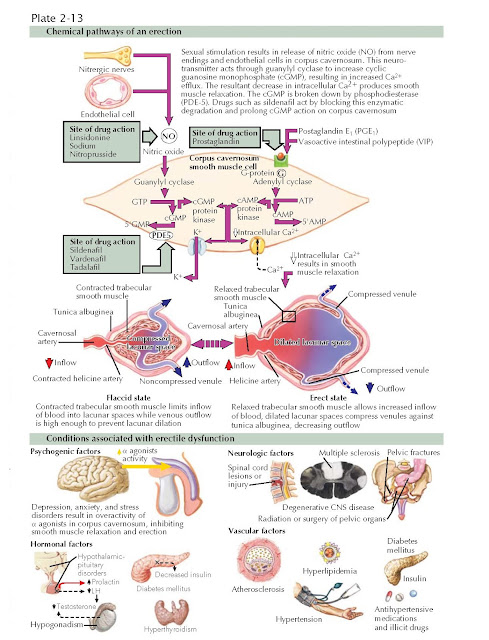
relaxing factors from penile endothelial cells result in an erection. Nitric
oxide released from parasympathetic nerve terminals is the principal
neurotransmitter for penile erection. Within penile smooth muscle, nitric oxide
activates a guanylyl cyclase that raises intracellular concentrations of cyclic
guanosine monophosphate (GMP). Cyclic GMP in turn activates cGMP dependent
protein kinase, which results in the opening of the potassium channels,
hyperpolarization, and sequestration of intracellular calcium. As a result of a
drop in cytosolic calcium, smooth muscle relaxation occurs, leading to
erection.
Subsequent
to the activation of this signal pathway, three events are required for a
normal erection: (1) relaxation of smooth muscle in the arteries and arterioles
supplying erectile tissue. This results in a several-fold increase in blood
flow. Concomitantly, there is (2) relaxation of the cavernous sinusoidal smooth
muscle within the paired corporeal bodies, facilitating rapid filling and
expansion of the sinusoids. As a result, (3) venous plexuses located between
the cavernous sinusoidal spaces and the tunica albuginea covering the corporal
bodies are compressed, resulting in almost total occlusion of venous outflow.
These events effectively trap blood within the corpora cavernosa and raise the
penis from a flaccid to an erect position (tumescence phase). Both masturbation and
sexual intercourse trigger the bulbocavernosus reflex (see Plate 2-11) that
causes the ischiocavernosus muscles to forcefully compress the blood-filled
corpora cavernosa. During ejaculation, penile intracavernous pressures reach
several hundred millimeters of mercury (rigid phase). During this phase,
vascular inflow and outflow temporarily cease. Detumescence results when erectile
neurotransmitter release stops, when phosphodiesterases break down second
messengers, or as a result of sympathetic discharge during ejaculation. On
return to the flaccid state, cyclic GMP is hydrolyzed to guanosine monophosphate
by phosphodiesterase type 5. Currently, three oral agents prescribed for
erectile dysfunction work by blocking phosphodiesterase enzyme activity.
Erectile Dysfunction
Erectile
dysfunction is traditionally classified as psychogenic or organic in nature.
Among organic forms, there are neurogenic, hormonal, arterial, venous, or
cavernosal and drug-induced. It is now clear that cardiovascular risk factors
suggestive of the “metabolic syndrome,” such as hypertension, dyslipidemia,
ischemic heart disease, and diabetes mellitus are associated with generalized
penile arterial insufficiency. In fact, significant erectile dysfunction precedes
heart attacks and stroke events by 5 to 7 years. Common causes of psychogenic
erectile dysfunction include performance anxiety, strained relationship, lack
of sexual arousability, and overt psychiatric disorders, such as depression and
schizophrenia. Neurologic disorders such as Parkinson and Alzheimer diseases,
stroke, and cerebral trauma can cause erectile dysfunction by decreasing libido
or affecting the cerebral control of erection. In men with spinal cord injury,
the degree of erectile function varies widely and depends on the lesion.
Hormonally, androgen deficiency causes a decrease in nocturnal erections and
decreases libido. Hyperpro-lactinemia of any cause results in sexual
dysfunction
because
of the inhibitory action of prolactin on gonadotropin-releasing hormone
secretion, resulting in hypogonadotropic hypogonadism. Sexual function also
progressively declines in “healthy” aging men. For example, the latent period
between sexual stimulation and erection increases, erections are less turgid,
ejaculation is less forceful, ejaculatory volume decreases, and the refractory
period between erections lengthens.
Erectile
Dysfunction Evaluation
Erectile
dysfunction can be the presenting symptom of various diseases. Therefore, a
thorough history (medical, sexual, and psychosocial), physical examination, and appropriate
laboratory tests aimed at detecting these diseases should be performed. The
physical examination should evaluate the breast, hair distribution, penis and
testis, femoral and pedal pulses, and testing of genital and perineal
sensation. Recommended laboratory tests include urinalysis, complete blood
count, fasting blood glucose, lipid profiles, and testosterone. The physician
should then assess the findings, inquire about the goals and preferences of the
man (and partner), and discuss therapeutic options. Cardiovascular risk factors
should be determined and an appropriate referral made if these risks exist. In
most cases, erectile dys unction can be treated with systemic or local therapy.


.webp)

