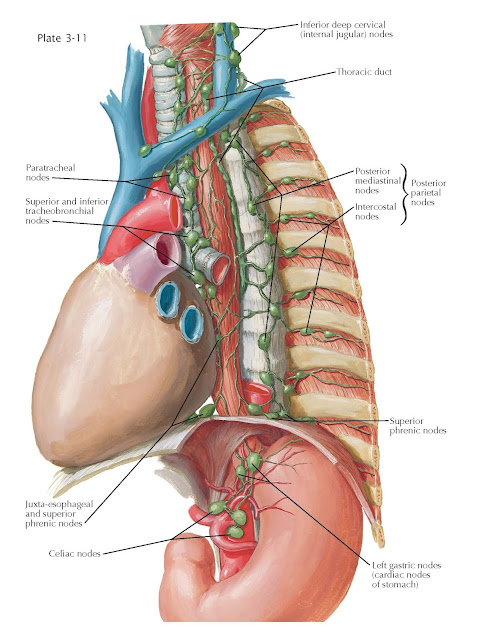
Lymphatic Drainage
of Esophagus
The esophagus contains a rich network of lymphatic vessels, largely in
the lamina propria of the mucosa but also in the other layers. From the cervical esophagus, lymph
vessels course chiefly to the inferior deep cervical (internal jugular)
lymph nodes and possibly also to the nearby paratracheal nodes situated
in the groove between the esophagus and trachea. The internal jugular lymph
nodes, a subdivision of the deep cervical nodes, lie along the internal
jugular vein, stretching from the parotid gland to the clavicle. On the left
side, they drain to the thoracic duct and on the right to the short right lymph
duct, which opens into the right subclavian vein at the angle formed by the
latter with the internal jugular vein.
From the thoracic esophagus,
lymphatic fluid drains posteriorly to the posterior mediastinal and intercostal
lymph nodes. The posterior parietal nodes are formed of the
posterior mediastinal and intercostal nodes. The posterior mediastinal nodes
lie alongside the vertebral column, and the intercostal nodes are in the nearby
intercostal spaces. Both these groups drain generally superiorly and eventually
empty into the thoracic duct or into the right lymph duct, which terminates at
the right subclavian vein, where it joins the right jugular vein. The superior
phrenic nodes near the posterior esophagus are closely associated with the
posterior parietal nodes, to which they drain. Anteriorly, the thoracic
esophagus drains to the paratracheal, superior tracheobronchial, and inferior
tracheobronchial lymph nodes; more inferiorly, lymphatic fluid drains to juxtaesophageal
and superior phrenic lymph nodes before flowing superiorly.
The paratracheal nodes form
a chain on each side alongside the trachea along the course of the recurrent
nerves. The superior and inferior tracheobronchial nodes
are the group that is situated about the bifurcation of the trachea and in the
angle formed by the bifurcation. These lymph nodes may be responsible for the
formation of traction diverticula when they become fibrosed as a result usually
of tuberculous involvement. The tracheal and tracheobronchial nodes drain
superiorly and usually form on each side a bronchomediastinal trunk, which, in
turn, joins either the thoracic duct or the right lymph duct. They may,
however, also have independent openings into the veins or may unite with the
internal thoracic chain or a low node of the internal jugular chain.
From the short abdominal portion of
the esophagus, lymphatic drainage is similar to that from the upper portion of
the lesser curvature of the stomach, chiefly to the cardiac nodes of the
stomach, which are a subdivision of the left gastric lymph node group. From
here, in turn, drainage is to the celiac lymph nodes. Some lymph vessels
from this region also pass superiorly through the esophageal hiatus of the
diaphragm and connect with the vessels and nodes above the diaphragm. Drainage
from the left gastric nodes is along the course of the left gastric artery and
coronary vein to the celiac nodes situated on the aorta in relation to the root
of the celiac trunk. These nodes, in turn, empty into the cisterna chyli
or the thoracic duct.


.webp)

