LICHEN PLANUS
Lichen
planus is a common inflammatory skin disease. It is unique in that it can
affect the skin, the mucous membranes, the nails, and the epithelium of the
hair follicles. Lichen planus most commonly affects the skin, but the other
areas can be involved either solely or in conjunction with one another. Lichen
planus that involves the skin has a tendency to spontaneously remit within 1 to
2 years after onset, whereas the oral version is almost always chronic in
nature.
Clinical
Findings: Lichen planus can affect people at any age, but it is much more common in
adulthood. It has no gender or racial predilection. The rash classically has
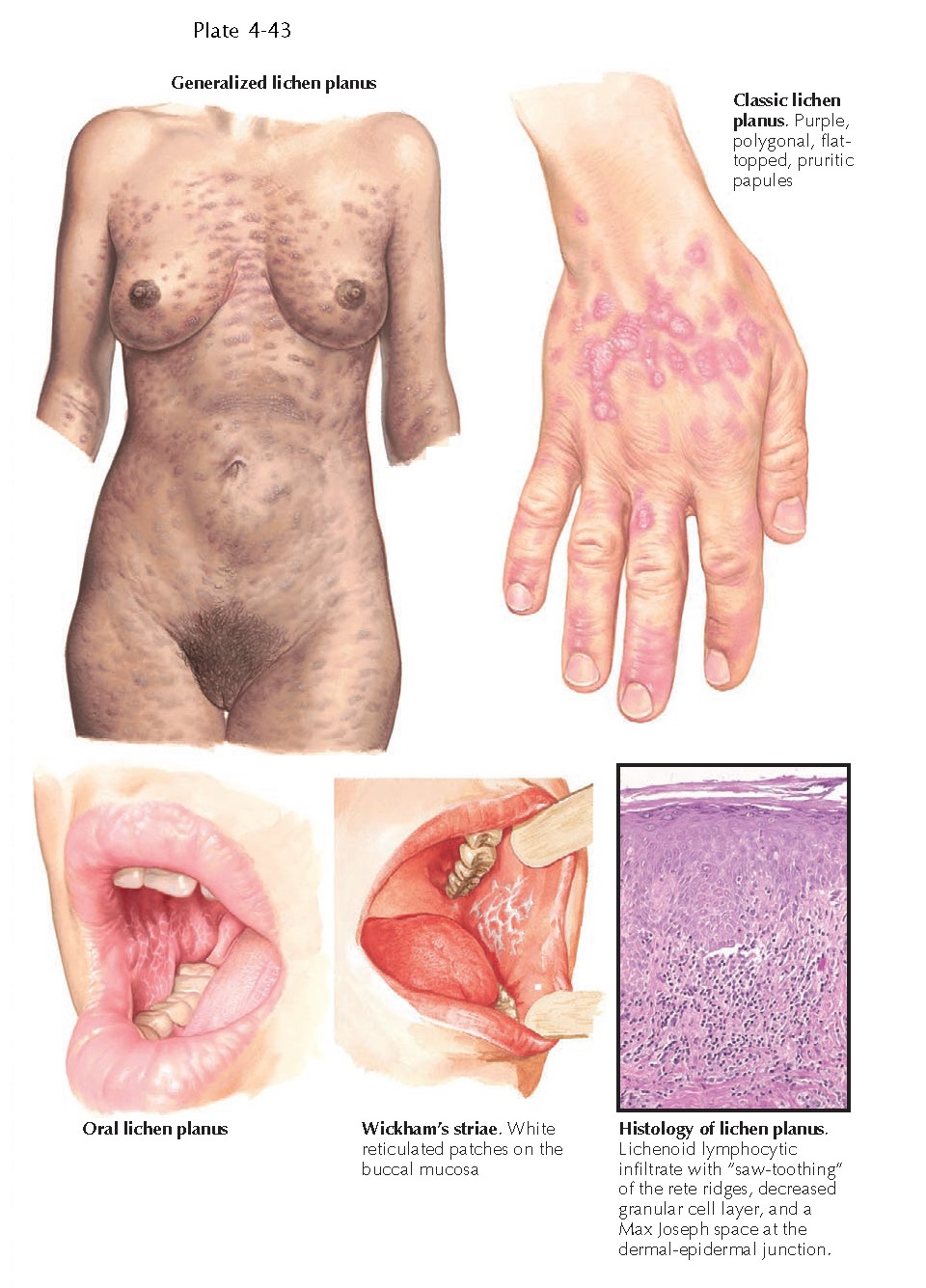
been described as flat-topped, polygonal, pruritic, purple papules. Frequently,
a whitish, lacy scale, referred to as Wickham’s striae, overlies the papules.
Lichen planus is unusual in that the pruritus causes the patient to rub the
area, rather than scratch. Lichen planus exhibits the Koebner phenomenon, and
often areas of linear arrangement are seen secondary to trauma or rubbing. This
is helpful when clinically examining a patient, because scratch marks and
excoriations are rarely seen, whereas lichenification from repeated rubbing of
the lesions is frequently seen. The rash has a tendency to be more prominent on
flexural surfaces, especially of the wrists. The glans penis is another
distinctive location in which lichen planus commonly occurs.
Many
clinical variations of lichen planus have been described. An afflicted
individual may have more than one morphology. Hypertrophic lichen planus has
the appearance of thickened, scaly plaques with a rough or verrucal surface.
There may be areas on the periphery that appear more classic in nature. This
variant can be difficult to diagnosis clinically, and often a biopsy is
required. It also can be difficult to treat effectively, and it runs a chronic
course. Rarely, hypertrophic lichen planus has been reported to transform into
malignant squamous cell carcinoma. Bullous lichen planus is an extremely
uncommon variant that usually occurs on the lower extremities. The vesicle or
bulla typically forms within the center of the lichen planus lesion.
Lichen
planopilaris is the term given to describe lichen planus affecting the terminal hair
follicles. This is most common on the scalp and leads to a scarring alopecia.
The typical findings are small, erythematous patches surrounding each hair
follicle. As the disease progresses, loss of hair follicles is observed,
signifying that scarring is taking place. The central crown is the area most
often affected. It is uncommon for the entire scalp to be affected. Once
scarring has occurred, the hair loss is permanent. Lichen planopilaris runs a
chronic waxing and waning clinical course.
Lichen
planus may affect the mucous membranes of the oral cavity, the genital region,
and the conjunctiva. These areas appear as glistening patches with lacy, white
reticulations on the surface. Mucous membrane lichen planus has a higher
tendency to ulcerate than the cutaneous form does. There have been reports of
malignant transformation to squamous cell carcinoma. For this reason, long-term
follow-up is required. Lichen planus may also affect the nail matrix and nail
bed, leading to dystrophy and nail abnormalities. The most frequently seen nail
abnormality is longitudinal ridging, but the most characteristic nail finding
is pterygium formation.
Pathogenesis:
Lichen
planus appears to be mediated by an abnormal T-cell immune response. The T cells
act locally on the keratinocytes to induce the clinical findings. The exact
pathomechanism has yet to be described.
Histology:
The
lesions show characteristic findings that include a dense lichenoid lymphocytic
infiltrate along the dermal-epidermal border. Necrotic keratinocytes are
frequently encountered within the hyperplastic epidermis and have been named
Civatte bodies. Hypergranulosis is a prominent feature as is the “saw- tooth”
pattern of epidermal hyperplasia. The presence of eosinophils should lead one to consider the
diagnosis of a lichen planus–like drug eruption or lichenoid contact
dermatitis.
Treatment:
Isolated
lesions can be treated with topical corticosteroids. Up to two thirds of skin
lesions resolve spontaneously. Patients with widespread disease present a
therapeutic challenge. Ultraviolet phototherapy, oral corticosteroids, and oral
retin ids such as acitretin
and isotretinoin have been used.


.webp)

