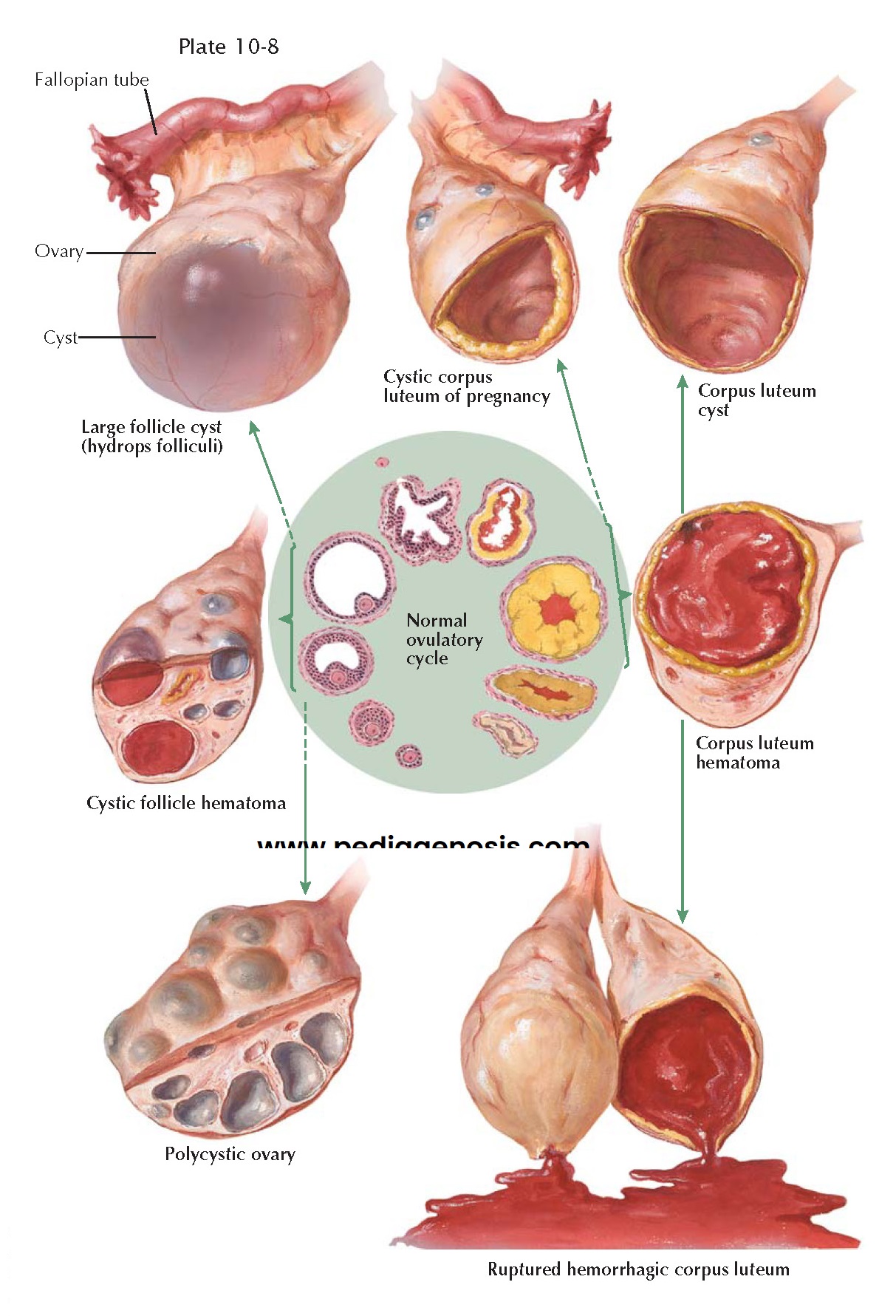
PHYSIOLOGIC VARIATIONS, NONNEOPLASTIC CYSTS
The preponderance of small cystic structures within the ovary represents physiologic variations of the normal ovulatory cycle. These follicle and corpus luteum derivatives are nonneoplastic, that is, they are incapable of autonomous growth. Their clinical recognition and differentiation from true ovarian cysts are most important. A small neoplastic ovarian cyst may be simulated by a single, large follicle cyst, by multiple cystic follicles, or by a corpus luteum cyst. A large or cystic corpus luteum of pregnancy may be mistaken for an ectopic pregnancy or an ovarian cyst. A corpus luteum hematoma may present with signs comparable to those associated with torsion of a small cyst. A ruptured graafian follicle or ruptured hemorrhagic corpus luteum may be misdiagnosed as acute appendicitis or ruptured tubal pregnancy. It is not uncommon to find adnexal cysts during pelvic ultrasonography performed for other reasons, and these are generally not of any clinical significance. Follicle cysts are distended atretic follicles more than 6 to 8 mm in diameter. They are usually not more than 1 to 2 cm in diameter, thin-walled, translucent, and filled with watery fluid. The cysts may project slightly above the surface of the ovary or may lie more deeply within the cortex. If pricked, the follicle fluid may spurt out under pressure. The inner lining appears smooth and glistening. Microscopically, the granulosa cell lining varies in thickness and may be well preserved or may show evidence of degeneration. On pelvic examination, a unilateral, smooth, cystic, slightly tender, movable, plum-sized ovary may be felt. Therapy is based on the principle that during the reproductive years a cystic ovary up to 6 cm in diameter is presumed, unless proved otherwise, to be a physiologic variation that will undergo subsequent resorption. The patient is reexamined at intervals. If the ovarian enlargement per- sists or increases in size, surgical intervention may be indicated.
The mature corpus luteum presents a central core filled with blood. With
resorption, the cavity may be distended with hemorrhagic or clear fluid, or
newly formed connective tissue. Variations in the size of the lumen occur normally.
A corpus luteum hematoma is the result of excessive hemorrhage into the corpus
cavity during the stage of vascularization. This increased accumulation of
blood under pressure may result in local pain, ovarian enlargement, and
tenderness. A corpus luteum cyst follows the resorption of a corpus luteum
hematoma. It is usually 2 to 4 cm in diameter. Grossly, the yellowish hue of
the cyst wall may be evident. A corpus albicans cyst is the sequel to a corpus
luteum cyst in which the lutein cells are replaced by a dense, wavy band of
fibrous or collagenous tissue.
A ruptured graafian follicle or hemorrhagic corpus luteum may be associated with varying degrees of intraabdominal bleeding. The former is likely to occur between the 12th and the 16th days and the latter during the last week of an average menstrual cycle. Rupture may occur spontaneously or may follow trauma, pelvic examination, coitus, or exercise. Symptoms and signs include lower abdominal pain, nausea and vomiting, abdominal spasm, tenderness and rebound tenderness, an enlarged, tender ovary, fullness in one adnexal region or the posterior cul-de-sac, and tenderness on manipulation of the cervix. The temperature may be slightly elevated and a leukocytosis may be found, but the leukocyte sedimentation rate remains normal. Ultrasonography will demonstrate the cystic mass and free fluid in the cul-de-sac. Mild cases may be confused with acute appendicitis or torsion. With bed rest the symptoms and signs gradually abate. If rupture is associated with severe bleeding, it may simulate a ruptured ectopic pregnancy. The blood loss, at times, may exceed 1000 mL.