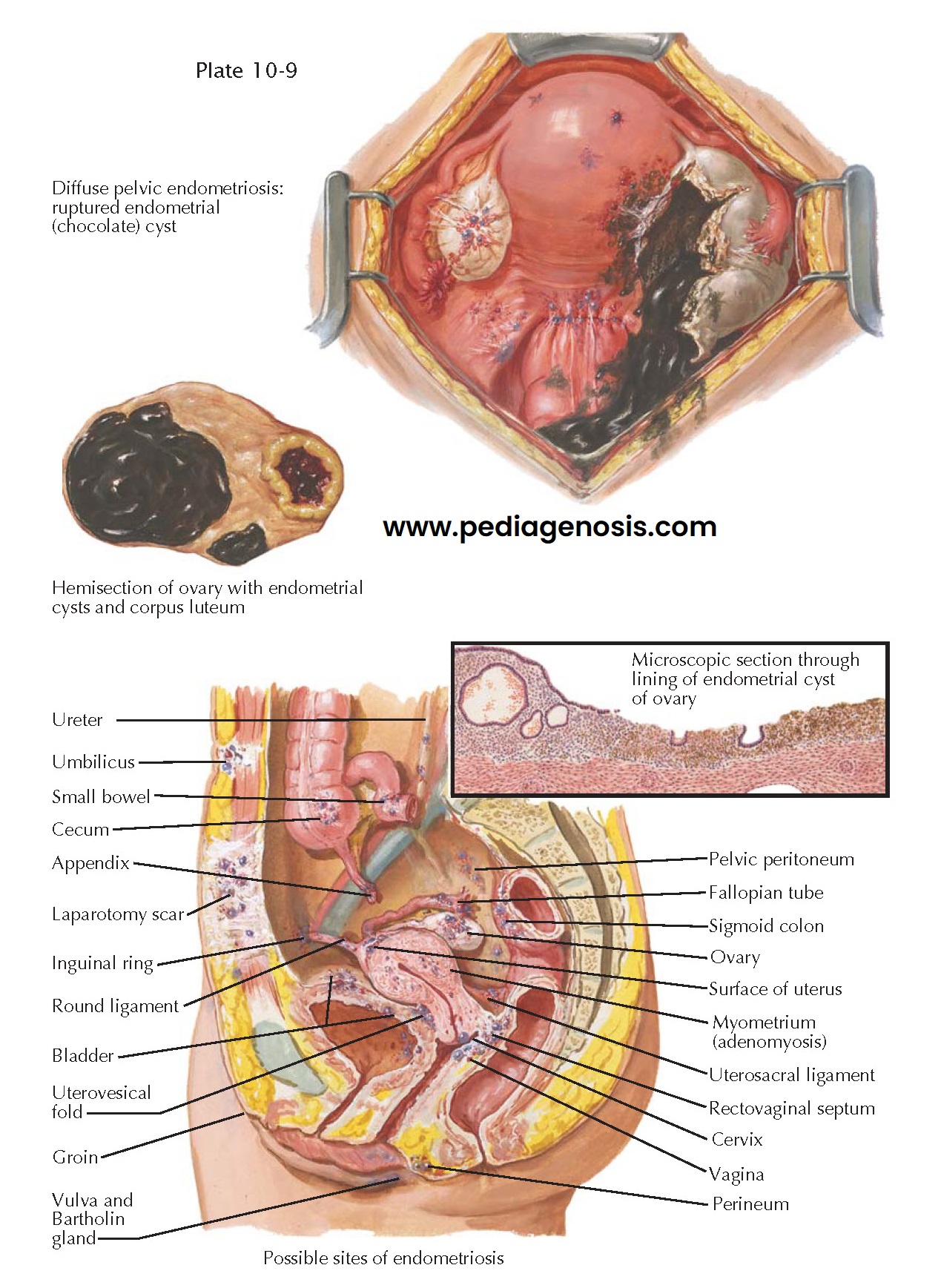
ENDOMETRIOSIS II—PELVIS
Endometriosis refers to the growth of endometrium outside of its normal intrauterine location (ectopic) that retains the histologic characteristics and biologic response of the endometrium. It is nonneoplastic, that is, incapable of autonomous growth, but it is dependent on estrogenic and progesterone stimulation. Endometriosis may arise by one of several proposed mechanisms—lymphatic spread, metaplasia of coelomic epithelium or müllerian rests, seeding by retrograde menstruation, or direct hematogenous spread. Instances of presumed iatrogenic spread (surgical) have been reported. A role for an immunologic defect is debated but remains to be conclusively established. The greatest incidence occurs between 30 and 40 years of age and may be found in 5% to 15% of women, 20% of gynecologic laparotomies, 30% of chronic pain patients, and 30% to 50% of infertility patients.
Small lesions may be asymptomatic (30%). The diagnosis may be suggested
by the presence of infertility, dysmenorrhea, sacral backache, deep thrust
dyspareunia, and abnormal uterine bleeding. Pain caused by endometriosis
characteristically begins premenstrually and ceases shortly after the menstrual
flow is established. Involvement of the rectovaginal septum, cul-de-sac, or
rectal wall may be responsible for rectal pain. If bowel endometriosis has
penetrated the intestinal wall, the rectum may bleed cyclically. Bladder
endometriosis may cause periodic hematuria and bladder irritability.
The presumptive diagnosis of pelvic endometriosis is based on the
history, the absence of a previous pelvic infection, and characteristic findings
on bimanual vaginal and rectal examinations. A final diagnosis requires
laparoscopy, laparotomy, or histologic confirmation. Pelvic examination may
reveal the presence of small, firm, tender, fixed nodules in the region of the
uterosacral ligaments, the posterior cul-de-sac, and the posterior surface of
the uterus. The uterus is not infrequently retroverted, retroflexed, and fixed.
Endometrial cysts are usually bilateral, rarely larger than a lemon or orange,
cystic, and firmly fixed behind the uterus.
At laparotomy, endometriosis may be found incidentally to other pelvic
lesions, particularly uterine fibroids and uterine retrodisplacements.
Peritoneal implants may be seen as small, scattered, scarred puckerings or
irregular, brown (“tobacco-stained”) areas anywhere on the pelvic peritoneum.
The peritoneum may be the site for atypical endometriosis, vesicles from clear,
to red, to the classic dark-brown lesion. The ovarian or uterosacral ligaments
may contain single or multiple discrete or confluent cicatrized nodules, with
partially enveloped, minute, dark-blue or brown hemorrhagic blebs.
Endometriosis of the ovary may be manifested by minute surface “implants,”
small hemorrhagic cysts within the cortex, or by large “chocolate” cysts, which
may practically replace the substance of the ovary. In surface endometriosis,
tiny red, purple, or dark-brown hemorrhagic blebs are encompassed within
puckered, cicatricial tissue. Endometrial cysts (chocolate cyst) vary in size
but are rarely larger than 10 cm in diameter. They are frequently bilateral. The
outer surface appears irregular, puckered, and adherent. Black or brown hem-
orrhagic areas may be evident. Along with its corre-sponding tube, the ovary
is usually found adherent to the posterior surface of the broad ligament,
uterus, lateral pelvic wall, and rectosigmoid. An attempt to free the adnexa
usually results in rupture of the cyst with escape of large quantities of
thick, chocolate-colored fluid. The cyst wall appears thick, irregularly convo-
luted, and yellow-white in color. The inner lining has a dark, hemorrhagic
stain. Microscopically, typical endometrial stroma and glands may line the cyst
wall. Older lesions, presumably due to repeated desquamation and pressure of
retained blood, may show little evidence of endometrial tissue. The cyst may be
lined by a broad zone of pseudoxanthoma cells, containing a hemoglobin
derivative (hemosiderin). Hyalinization and fibrosis are seen in other areas.
Therapy depends upon the age, parity, location, and extent of the lesions, severity of symptoms, the desire for children and the possibility of pregnancy, the patient’s attitude toward loss of menstrual function or premature castration, and the coexistence of other pelvic pathology such as uterine fibroids.