STROMATOGENOUS NEOPLASMS
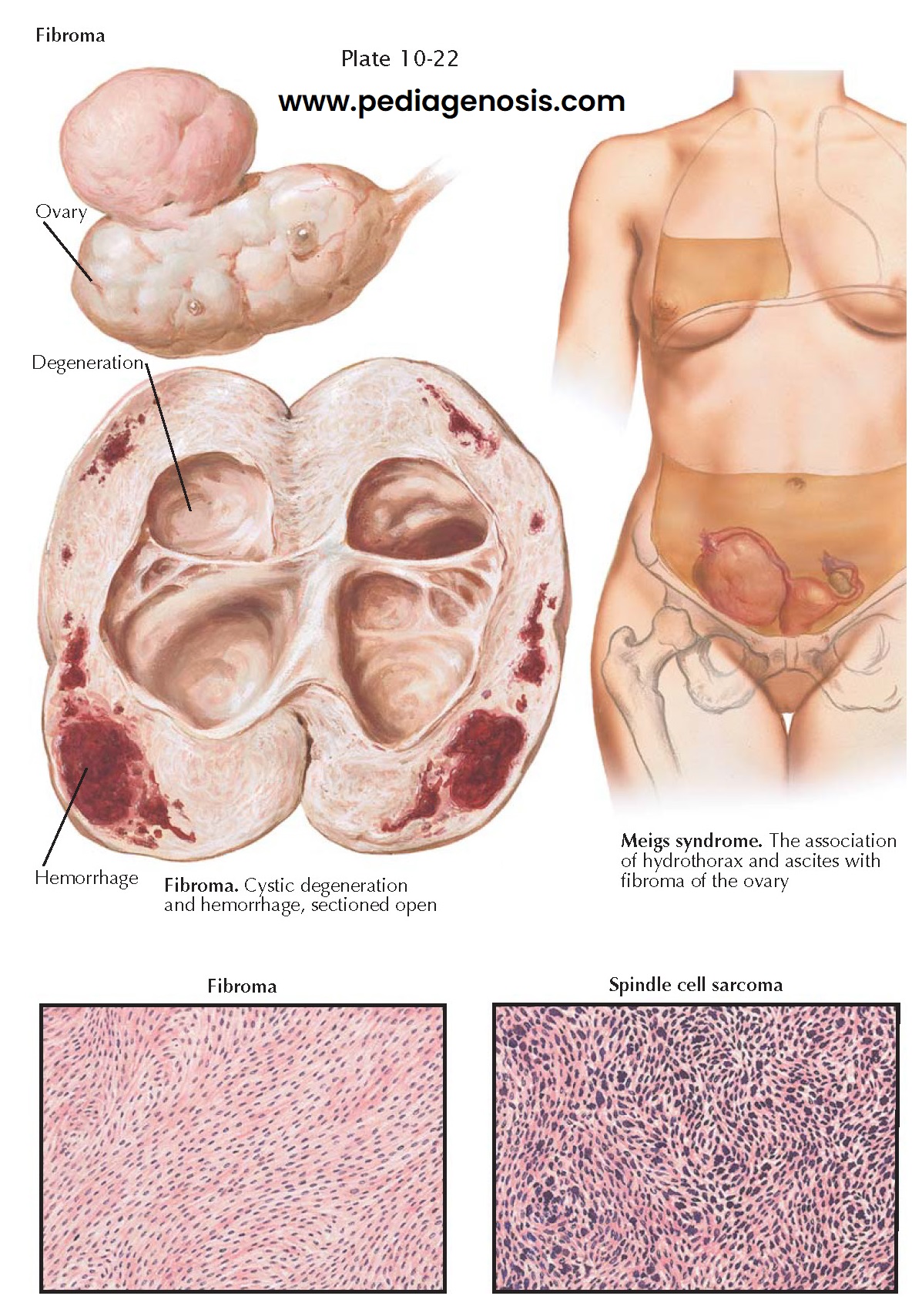
Ovarian fibromas are benign stromatogenous tumors. The most common benign ovarian tumor, this tumor is composed of stromal cells (fibroblasts). Although benign, these tumors are sometimes associated with ascites and hydrothorax (Meigs syndrome, 1% of patients). They may be minute or may reach a diameter of more than 27 cm. Unilateral involvement is usual (90%). Multiple fibromas of a single ovary occur occasionally (10%). Though encountered at any age, the majority are found postmenopausally. Because of its weight, torsion of the pedicle is apt to occur.
Fibromas are well-encapsulated, solid, heavy, oval, grayish-white tumors
with an irregularly bossed, smooth surface. Adhesions may be present. The cut
surface discloses dense, white, interlacing bundles of connective tissue. The
larger neoplasms may show focal or diffuse areas of edema, hemorrhage,
degeneration, and cyst formation. The cystic cavities result from tissue
necrosis and may be irregular or ragged and filled with clear or blood-tinged
fluid. Isolated or diffuse calcification occurs in 10% of cases. Microscopically,
the tumor is composed of interlacing strands or whorls of spindle-shaped cells.
The individual cell presents an indistinct border, a moderate amount of finely
granular cytoplasm, and an elongated, deeply stained nucleus. In the larger
fibromas, circulatory deprivation may result in edema, hemorrhage, infarction,
degeneration, necrosis, and calcification. In edematous areas, the cells are
widely separated and stellate in appearance. Dilated lymphatic channels may be
conspicuous. Hyalinization is evidenced by the deposition of pink-staining
homogeneous collagenous material. Phagocytic cells containing fatty material
may be seen in areas of necrosis. Infarction may be manifested by a diffuse
infiltration with erythrocytes, degeneration, and necrosis. Calcification is
indicated by the deposition of granules or masses of darkly stained basophilic
material.
If small, an ovarian fibroma may be asymptomatic. Those of larger size may
give rise to localized discomfort or pain, pressure symptoms, and abdominal
enlargement. The presence of a unilateral, hard, movable ovarian tumor with
ascites, or ascites and hydrothorax, is most suggestive. Therapy for ovarian
fibroma is surgical extirpation.
Meigs syndrome refers to the association of ascites and hydrothorax with
a pelvic neoplasm, particularly ovarian fibromas. The syndrome has also been
encountered with fibroadenomas, fibrosarcomas, Brenner tumors, theca cell tumors,
teratomas, serous cystadenomas, multilocular pseudomucinous cystadenomas,
adenocarcinomas, papillary cystadenocarcinomas, and even fibromyomas of the
uterus. Ascites is present with the majority of ovarian fibromas of moderate or
large size (40% if the tumor is >10 cm.). The right side of the chest is
involved in 75% of cases, the left in 10%, and both in 15%. No relationship
between the side of the ovarian tumor and the side of the hydrothorax seems to
be apparent. Varying amounts of fluid may accumulate rapidly in the peritoneal
and pleural cavities. The pathophysiology of ascites in Meigs syndrome is speculative.
The hydrothorax and hydroperitoneum disappear completely with removal of the
pelvic tumor. Differentiation must be made from a malignant tumor with
pulmonary metastases, cardiac or renal disease, hepatic cirrhosis, and
tuberculous peritonitis.
Fibrosarcoma of the ovary is extremely rare. It is usually unilateral,
solid, irregular, pedunculated, and of variable size. The cut surface may
present a variegated appearance, depending upon its cellularity and the
tendency to hemorrhage, necrosis, and cystic degeneration.
Areas may be gray-white or pink-tan in color, sometimes suggesting raw pork. Histologically, it may resemble a cellular fibroma or a solid, anaplastic carcinoma. It includes spindle, mixed, or round cell varieties, with irregular hyperchromatic nuclei and giant cells. The symptomatology is not distinctive. Torsion and ascites may occur. Extension may be by direct invasion or through vascular channels. If unilateral, encapsulated, and of low-grade malignancy, the prognosis following surgery is relatively good; otherwise it is poor.


.webp)

