DYSGERMINOMA, BRENNER TUMOR
The dysgerminoma is an ovarian tumor made up of germ cells and stroma that appear analogous in structure to the seminomas found in the male testes. Although rare, these tumors are the most common malignant germ cell tumors (1% to 2% of ovarian malignancies). At times, they may be associated with evidence of sexual underdevelopment or pseudoher-maphroditism. Although found at all ages, at least 75% of cases occur in young individuals between 10 and 30 years of age. Unilateral involvement is usual (90%).
The clinical manifestations of dysgerminoma are those associated with any
pelvic neoplasm. Tumor degeneration may induce a low-grade fever, leukocytosis,
and a rapid sedimentation rate. Ascites is not infrequent. Torsion with
infarction may occur (5%). Dysgerminomas usually grow rapidly. Extension takes
place by perforation of the capsule with direct infiltration, by peritoneal
spread, and by lymphatic and hematogenous routes. These tumors tend to spread
by lymphatic channels. Recurrence of tumor is found in 20% of patients, but
recurrent disease generally responds well to additional surgery, chemotherapy,
or radiation. The prognosis is good for patients with pure dysgerminomas less
than 15 cm in size. With limited disease and no indication of spread at the
time of surgery (stage I), there is a 90% 5-year survival rate.
Grossly, the dysgerminoma is a solid, round, oval, or irregular tumor,
which may vary in diameter from 3 to 5 cm or may fill the entire pelvis. It may
be firm and rubbery or soft and pliable. The cut surface is grayish, cellular,
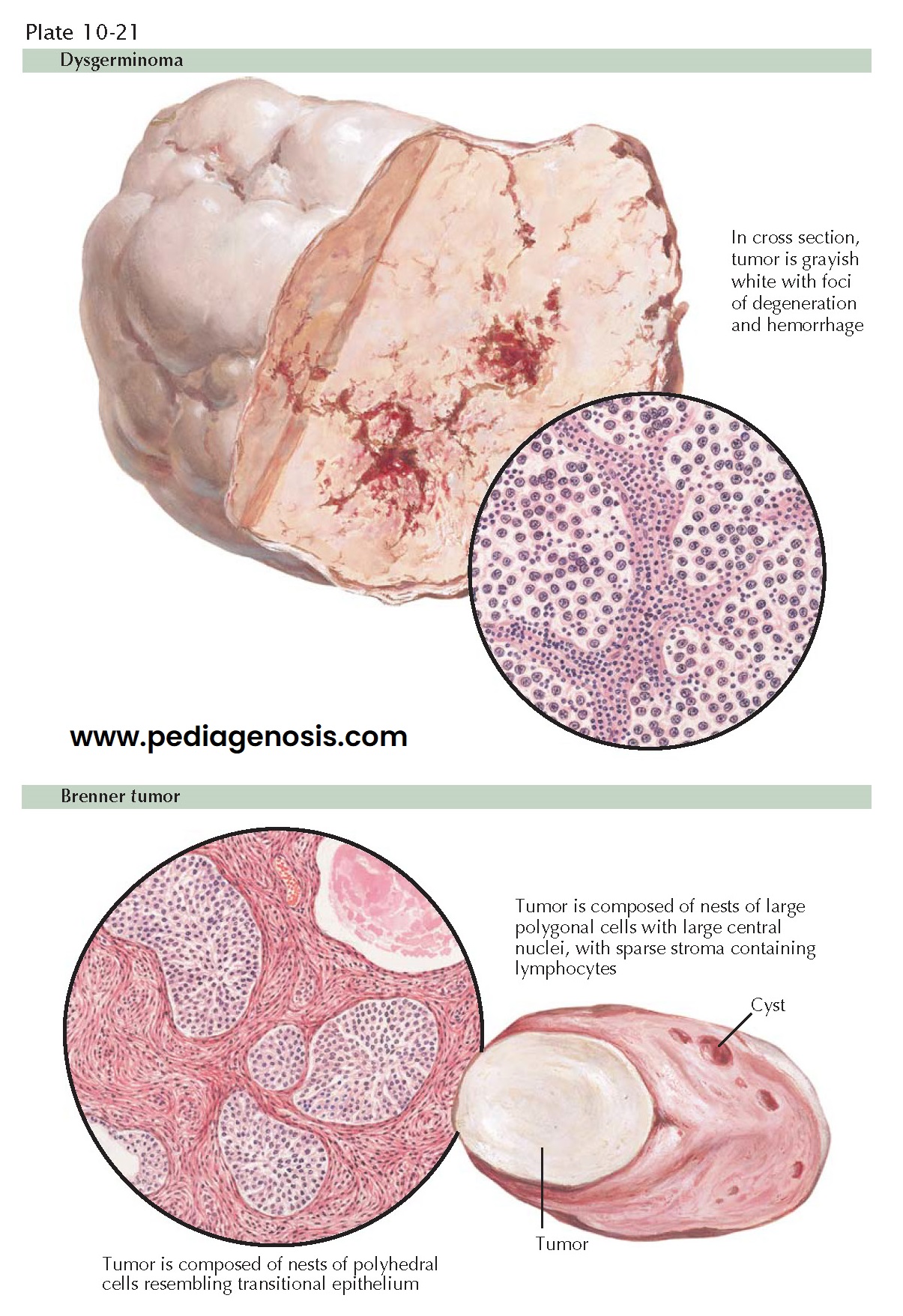
and, at times, brainlike. Usually, there is degeneration, necrosis, hemorrhage
and cavitation. Histologically, columns or nests of the characteristic cells
are separated by strands or trabeculae of loose, edematous, vascularized,
connective tissue that shows hyalinization and infiltration with lymphocytes. The
dysgerminal cells are large, sharply defined, round or polygonal, with centrally
placed, round, uniform nuclei. The cytoplasm is abundant, clear, or finely
granular. The nuclei are fine and diffuse, with prominent nucleoli. Mitoses may
be present. Foci of degeneration and necrosis, with foreign-body giant cells,
are common.
The transitional cell (Brenner) tumor is an epithelial tumor that is made
up of cells that resemble urothelium and Walthard cell nests, intermixed with
the ovarian stroma. Most are benign. It is relatively uncommon, comprising
about 1% to 3% of all ovarian neoplasms. The majority are encountered after 40
years of age or postmenopausally. At times, a small Brenner tumor may be found
incidentally in the wall of an ovarian cyst, usually of the mucinous variety.
Clinically, there are no characteristic features. Rarely, it is associated with
Meigs syndrome. At laparotomy, it may be difficult to differentiate a Brenner
tumor from an ovarian fibroma, fibromyoma, theca cell tumor, or adenofibroma.
Brenner tumors may be microscopic in size or may vary from a few to 13 cm
in diameter. They are unilateral, solid, round or oval, irregularly bossed,
smooth, firm, and grayish white in color. On section, the tumor appears well
demarcated, resembling a fibroma. Multiple, minute cystic spaces may be evident,
containing viscid, opaque, yellow-brown fluid.
Histologically, irregular masses or columns of polyhedral cells are surrounded by rather dense, fibrous tissue. The epithelial cells are large, irregular, polyhedral, or oval in shape, with distinct cell membranes. The cytoplasm is abundant, granular, and vacuolated. The nuclei are oval or slightly irregular, with distinct chromatin granules. Longitudinal nuclear grooving, representing a linear deposit of chromatin, may be seen. Microscopic cysts in the cell masses may be solitary or multiple. These are lined by flattened or cuboidal cells or by columnar epithelium containing glycogen and secretory granules that take a mucicarmine stain. The connective tissue about the epithelial strands is cellular, hyalinized, and avascular. Irregular, calcified deposits may be present.


.webp)

