ENDOCRINOPATHIES II—POLYCYSTIC OVARY SYNDROME
In 1935, Stein and Leventhal described a group of patients in whom the symptoms of amenorrhea, sterility, slight hirsutism, and occasional obesity were associated with the presence of bilaterally enlarged, polycystic ovaries. The syndrome is now known as polycystic ovary syndrome (PCOS). The exact pathophysiology of PCOS is not well established, but increased amplitude of gonadotropin-releasing hormone (GnRH) pulsation and abnormal secretion of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) during puberty are thought to result in androgen excess. Elevated levels of LH persist and may be used to help establish the diagnosis. Insulin resistance is a prominent aspect of this syndrome (40% of patients). It is clear that there is a genetic predisposition to PCOS; however, it is likely that several genes are involved.
The syndrome is not infrequent: up to 5% of women and 30% of secondary
amenorrhea cases. It is the most common hormonal disorder among women of
reproductive age. A consensus conference has defined PCOS as having two of the
following three: irregular cycles, clinical or biochemical evidence of
hyperandrogenism or polycystic appearing ovaries on ultrasound, as well as no
evidence of another cause of anovulation. The patient usually presents because
of infertility or secondary amenorrhea. Some degree of virilism is evident in
70% of cases. Hirsutism may be minimal or conspicuous, involving the face,
chest, breasts, and extremities, with male escutcheon. Generalized obesity has
been noted in 50% of cases. On pelvic examination, the ovaries are
symmetrically enlarged to the size of golf balls. The uterus may be
hypoplastic. Endometrial biopsy will usually reveal a proliferative phase.
Elevated levels of LH may be used to help establish the diagnosis. (A 2:1 ratio
of LH to FSH is considered diagnostic.) Patients suspected of having adrenal
sources of hyper-androgenism can be screened for adrenal hyperactivity by
measuring 24-hour urinary free cortisol, an adreno-corticotropic hormone (ACTH)
stimulation test, or an overnight dexamethasone suppression test. Serum
testosterone (total) is generally 70 to 120 ng/mL and androstenedione is 3 to 5
ng/mL. Dehydroepiandrosterone sulfate (DHEA-S) is elevated in roughly 50% of
patients. Ultrasonography (abdominal or transvaginal) may identify ovarian
enlargement or the presence of multiple small follicles. Magnetic resonance
imaging or computed tomography may be used to evaluate the adrenal glands.
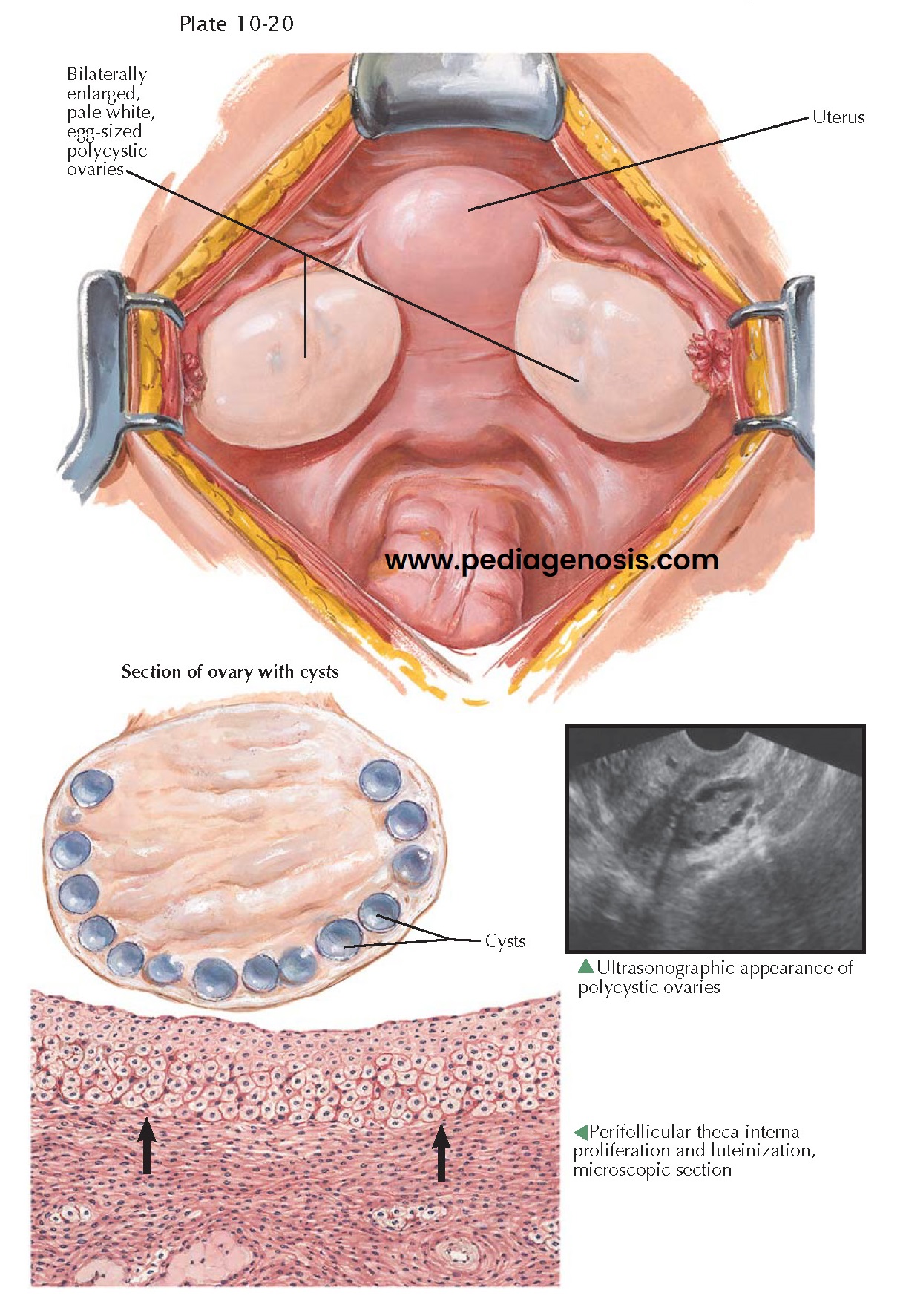
Grossly, the ovaries are conspicuously and symmetrically enlarged. They
may be two to five times normal in size, round or oval in shape, and gray white
or pearly white in color. The ovarian surface is smooth, with occasional slight
elevations, suggesting the presence of underlying cystic follicles. At times,
the gonads may be slightly flattened (“oyster” ovaries), or one may be slightly
larger than the other. On section, the tunica albuginea usually appears
thickened. Beneath it, numerous cystic follicles, 2 to 15 mm in diameter, ring
the cortex. The ovarian parenchyma is conspicuously hypertrophied and may
contain occasional yellow flecks. Microscopically, the important features relate
to the presence of a hyperthecosis. Around many of the atretic cystic
follicles, the theca interna layer shows marked proliferation and
luteinization. The ovarian parenchyma appears hyperplastic, with evidence of
increased cellularity. Many of the cells are more epithelioid in appearance. Small
groups of luteinized cells may be seen scattered throughout the parenchyma.
Medical therapy has replaced surgical treatment. Treatment depends on the
desire for pregnancy; if pregnancy is desired then ovulation induction may be
required. Weight loss is often associated with resolution of symptoms and a
return of menstrual function in patients with mild or early polycystic ovary
disease. Combination oral contraceptives (50 g [microgram] formulation and a
progestin other than norgestrel) may reduce further hair growth. If DHEA-S is
elevated, dexamethasone may be added to oral contraceptives. Metformin (1500
mg/day) is often used as an adjunctive treatment for ovulation induction and is
now considered as first-line therapy for PCOS.
There is an increased risk of diabetes, endometrial hyperplasia, and endometrial carcinoma in patients with polycystic ovaries and chronic anovulation.


.webp)

