INTERTROCHANTERIC FRACTURE OF FEMUR
Intertrochanteric
fractures of the femur typically occur in persons 10 years older than those who
sustain fractures of the femoral neck. These fractures occur along a line that
connects the greater and lesser trochanters. Fractures can result in a simple
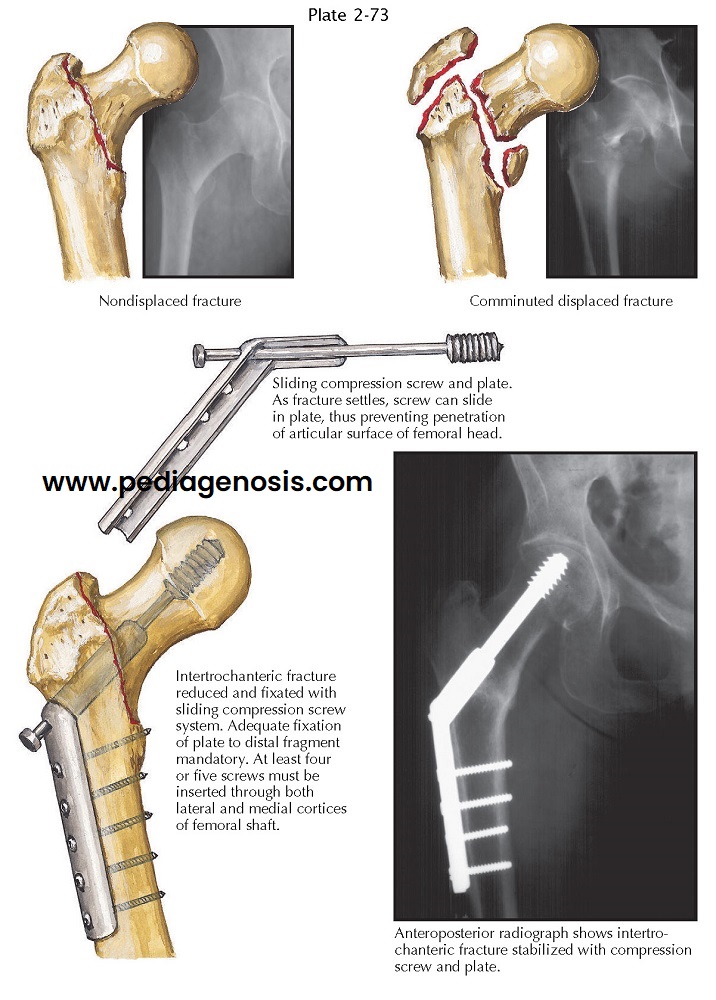
two-part displacement or in more complex, comminuted fractures. Because the
fracture surfaces created in the injury are large and filled with an abundance
of cancellous bone, delayed union or nonunion is rare. Although nonoperative
treatment with prolonged bed rest can be employed, the fractures are most
commonly treated with ORIF.
Of the many classifications of intertrochanteric fractures, the system developed by Evans appears to be the most useful for selecting appropriate treatment. The fractures are classified into two types, stable and unstable. The system is based on whether a stable reduction of the fracture at the medial and posteromedial aspects of the fracture surface can be achieved. If stability is attained at these two sites, the fracture is likely to heal in this position with proper fixation. Evans noted that if stability could not be achieved, patients more frequently experienced loss of fixation or loss of reduction due to collapse of the fracture into a varus and externally rotated position.
The sliding compression screw was developed to treat intertrochanteric fractures of the femur. The unstable fracture fragments telescope along the sliding portion of the device to a position of stability. The screw portion of the device is securely fixated in the femoral neck and head, and the sliding portion allows for a controlled collapse of the fracture. Recent studies have demonstrated that use of the device has reduced the incidence of complications after surgical treatment of unstable intertrochanteric fractures. However, many surgeons prefer to achieve a stable reduction of the fracture before using any device to fixate it. Stable fixation lessens the stresses applied to the sliding compression screw, which decreases the risk of implant failure. Postoperative management depends on the patient’s ability to cooperate with a rehabilitation program, the quality of the bone in the proximal femur, and the adequacy of the reduction and fixation. Cooperative patients with good-quality bone and secure fracture fixation can be mobilized early with progressive weight bearing. Uncooperative patients or those unable to understand the postoperative treatment program are mobilized more slowly and cautiously. At first, these patients are simply moved from bed to chair. A similar postoperative program is recommended for patients with poor-quality bone and for those with markedly comminuted fractures and fracture instability. Comminuted intertrochanteric fractures may require bone grafting at the time of fracture fixation.


.webp)

