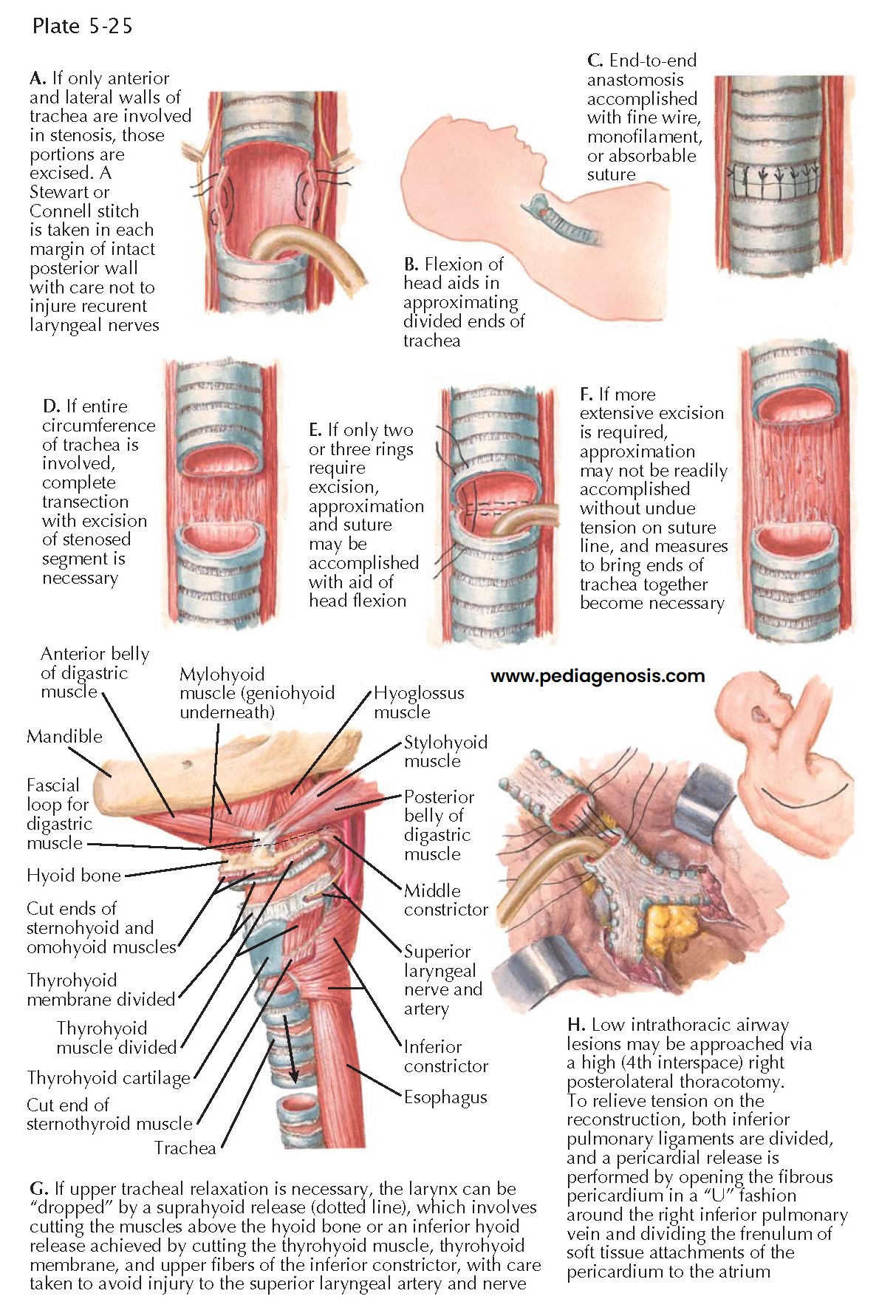
TRACHEAL RESECTION AND ANASTOMOSIS
Tracheal stenosis can be idiopathic but is most commonly the result of prior intubation or tracheostomy. Common areas of stenosis were previously located in the mid-trachea related to high-pressure, low-volume endotracheal tube cuffs; however, contemporary endotracheal appliances have low-pressure cuffs. Today stenotic lesions are typically found in the proximal or subglottic trachea at the site of a prior stoma. Mid- to distal tracheal resections are more likely performed as therapy for benign or malignant airway tumors. In most cases of symptom-producing stenosis of the trachea, conservative therapy, consisting of repeated dilatations, is either contraindicated or has proven to be ineffective. Consequently, surgical correction is necessary. The procedure of choice is resection of the stenotic tracheal segment with primary reconstruction via an end-to-end anastomosis (see illustration).
Resection and primary reconstruction are more easily
accomplished if the lesion is in the cervical portion of the trachea than if it
is within the mediastinum. In the former instance, the approach is via a transverse
cervical incision; in the latter case, a full or partial (upper) median sternotomy
or a fourth intercostal space right posterolateral thoracotomy may be required.
Low intrathoracic tracheal lesions are more easily approached through a posterolateral
thoracotomy, although some surgeons prefer a transpericardial approach accessing
the trachea and main carina between the ascending aorta and superior vena cava through
a sternotomy. Preoperative study of the location and extent of the lesion using
both fiberoptic bronchoscopy and computed tomography is essential; the situation
must be further evaluated at the time of surgery. Usually, the stenotic segment
may be identified by the “hourglass” constriction of the outer tracheal wall. Nevertheless,
the lumen must be examined via a transverse incision at the lower end of the constriction
to determine whether the stenosis is circumferential or confined to the anterior
and lateral cartilaginous walls of the trachea. Only the diseased region of the
trachea should be dissected circumferentially to preserve the segmental
blood supply of the remaining airway. For benign diseases, dissection should be directly on the airway cartilage to prevent injury to the recurrent laryngeal nerves that pass nearby in the tracheoesophageal groove. As the anastomosis is being completed, the surgeon assesses the reconstruction for tension. The patient’s intraoperative position is adjusted by the anesthetist from full extension to partial neck flexion with pillows and blanket rolls to support the head. Additional length can be gained via release maneuvers. For extensive proximal tracheal resections, a suprahyoid or infrahyoid release may facilitate approximation of the divided tracheal ends. To relieve tension on an intrathoracic reconstruction, these cervical maneuvers provide minimal additional length. Releasing one or both inferior pulmonary ligaments as well as incision of the right-sided pericardial attachments to the atrium and inferior pulmonary vein is more efficacious.