FROZEN SHOULDER
The
clinical and anatomic pathology in frozen shoulder is derived from an acute
inflammatory synovitis followed by an intracapsular soft tissue fibrosis,
resulting in contracture of the capsule.
Some have made an analogy of frozen shoulder to
Dupuytren contraction in the palmar fascia of the hand. Dupuytren contracture
has been associated with myofibroblasts present within the fibrous tissues, and
these same cells can be found in the shoulder capsule with frozen shoulder.
Frozen shoulder is commonly seen in association with thyroid disorders as well
as diabetes. Patients with these associated systemic diseases often have a more
severe and refractory clinical course. When associated with thyroid and
diabetic changes, the treatment of frozen shoulder is often more difficult. The
recovery phase is longer and protracted, and the recurrence rate and the number
of treatment failures are higher with both surgical and nonsurgical treatment.
There is a role for intra-articular
therapy with a corticosteroid, particularly in the treatment of early stages
of frozen shoulder in which there is acute inflammation of the synovium. As the
disease progresses through the second stage with more fibrosis and fewer
inflammatory changes, corticosteroid injections appear to have less of a
clinical effect. Nonsurgical treatment is focused on passive range of motion
stretching exercises that should take into account all portions of the capsule
and affect all arcs of motion to include forward flexion, abduction, and internal
and external rotation exercises. In many cases, the patient’s shoulder symptoms
are accompanied by significant pain, and as such the exercise program needs to
be performed gently but on a daily basis. Home-based exercise programs
instructed by a physical therapist are preferred. Stretching exercises in phase
I and phase II are shown later in discussion on rehabilitation. Home exercises
should be done daily and frequently for short periods of time. Typically, each
exercise session should include five of the types of stretches shown later in
the rehabilitation discussion each for 2 minutes, for a total of 10 minutes of
exercise at regular intervals at least five times per day. Persistence with
this regimen accompanied by good pain management will generally result in
significant improvement after 6 to 8 weeks. When pain is diminished and range
of motion near 80% of normal, a strengthening program can be added to the
overall program and the frequency of the stretching program can be diminished
and the length of time for each session increased to 15 to 20 minutes three
times each day.
In a small percentage of patients with
refractory clinical symptoms associated with significant loss of passive arcs
of motion, surgical management can be very effective. Idiopathic frozen
shoulder (adhesive capsulitis) is most responsive to both nonoperative and
surgicalmanagement as defined previously. Arthroscopic capsule release
involving all portions of the capsule is an effective mechanism to release the
contracted tissue and allow for ease of movement and postoperative
rehabilitation. Postoperative pain management should include consideration of
regional blocks. As with all types of treatment, pain management is important
and supports an effective postoperative rehabilitation program.
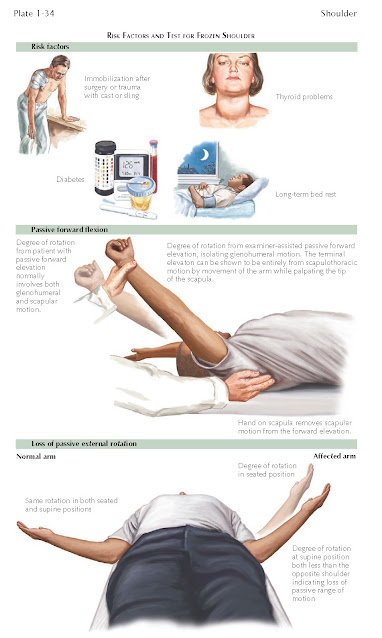
Examination of the frozen shoulder can
demonstrate loss of passive range of motion of the shoulder and is best tested
in the supine position as shown in Plate 1-34. As the examiner tries to further elevate the
arm, the examiner’s hand realizes loss of glenohumeral motion, and the terminal
phases of elevation are entirely related to scapular thoracic movement. In
addition, loss of passive external rotation can be seen in both the supine as
well as the seated position, as shown in Plate 1-34. Motion should be tested for both passive and
active range of motion. Loss of active range of motion in the setting of normal
passive motion is often related to weakness secondary to rotator cuff function
(see Plates 1-38, 1-40, and 1-43).



.webp)

