INFERTILITY I—CAUSES
Under ordinary circumstances, 80%
to 90% of normal couples conceive during 1 year of attempting pregnancy and 92%
to 95% will conceive within 2 years.
Infertility is defined as the inability to conceive despite more than 1 year of unprotected intercourse. This interval is reduced to 6 months of contraceptive-free intercourse if the woman is older than 35 years. Infertility may be subdivided into primary and secondary types based on the patient’s past reproductive history: nulligravida women, and men who have not fathered a child, are in the primary infertility group; those who have become pregnant or fathered a child, regardless of the outcome of that pregnancy, are in the secondary infertility group. (Infertility affects two individuals, but the classification is generally based on the woman’s history, with less emphasis on the male partner’s reproductive history.) Slightly more than one-half of infertility patients fall into the primary group. It is estimated that infertility impacts 6.1 million couples in the United States. The prevalence of infertility increases with the age of the woman, and age-related infertility is becoming more common because about 20% of American women delay their attempts at pregnancy until after age 35. The effect of age upon men’s fertility is less clear but evidently much less pronounced.
Multiple factors can contribute to the inability to conceive and deliver a
child. Conception requires the presence of competent gametes brought together at
an appropriate time to allow fertilization. Once fertilization occurs, the fertilized
ovum must be transported to an appropriately prepared uterine cavity where it
must be able to implant and grow. This growth must be supported by a functioning
corpus luteum until the placenta can take over hormonal support of the pregnancy.
To deliver a child, the developing embryo must still successfully grow, differentiate,
and transition to fetal state and grow to viability. The failure of any of
these steps may result in infertility (or recurrent preg- nancy loss).
The male partner of a couple attempting pregnancy must bring to the union
competent sperm. Approximately 35% to 50% of infertility is due to a male factor,
such as azoospermia (no spermatozoa). Problems with the production or delivery of
competent sperm can arise from genetic, central, or peripheral causes as dis-
cussed later (see the Infertility III section).
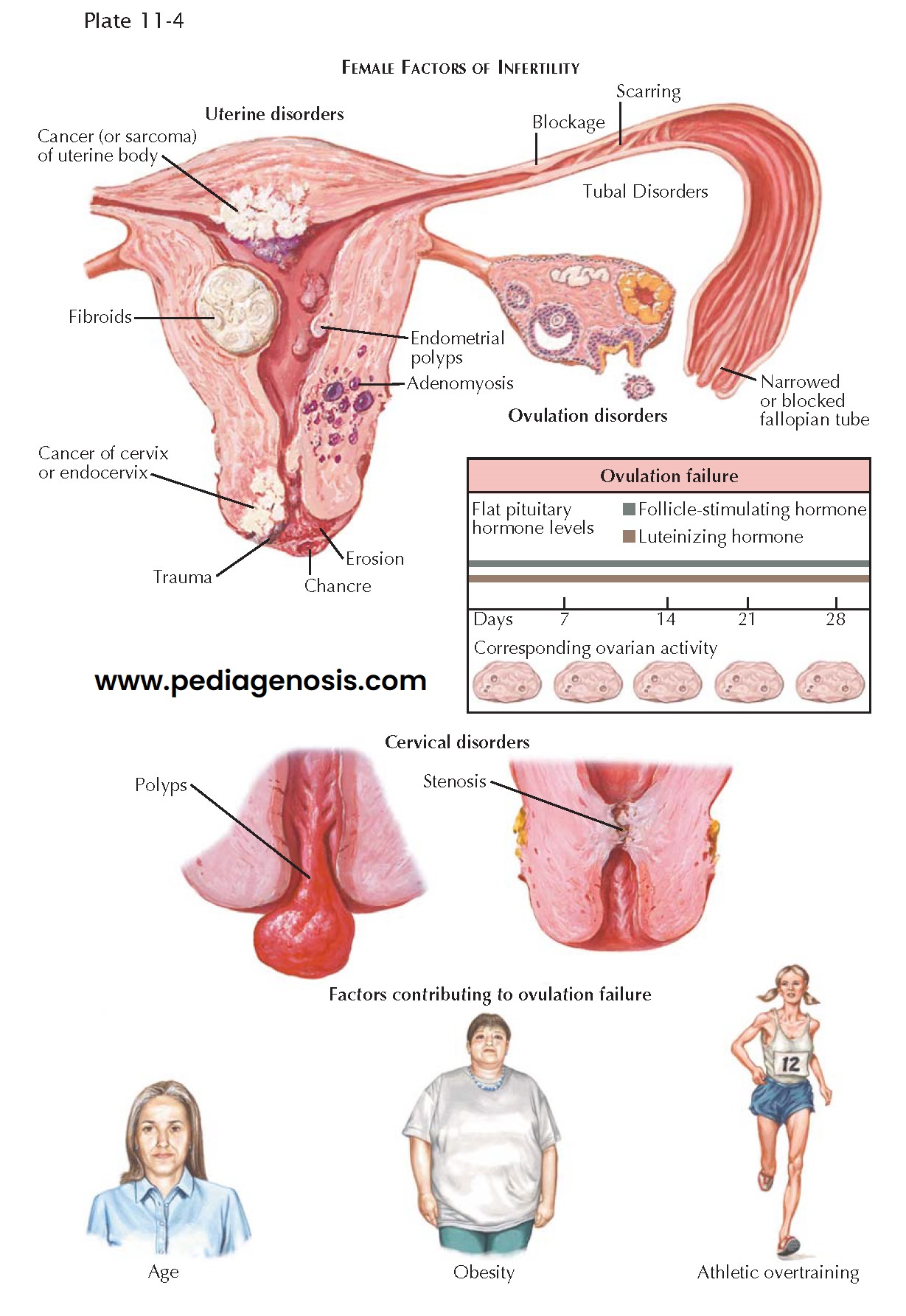
Female factors, such as tubal disease (20% to 30%), ovulation disorders (10%
to 20%), and cervical factors (5%), contribute to roughly 50% to 60% of female
causes. The remaining 10% to 20% of couples have no identifiable cause for their
infertility (idiopathic). Couples experiencing primary infertility are more likely
to have idiopathic or chromosomal causes than are couples that have conceived previously.
Factors that increase the risk of anovulation (obesity, athletic over-training,
exposure to drugs or toxins), the risk of pelvic adhesive disease (infection, surgery,
endometriosis), impaired sperm production (mumps, varicocele), or sperm delivery
(ejaculatory dysfunction) all may increase the risk of infertility. In many cases,
processes that impede fertility may not have an obvious clinical antecedent: half
of all women found to have tubal factor infertility have no history of antecedent
infections or surgery.
The evaluation of infertility is discussed further sub-sequently, but it is important to recognize that the process of evaluation can be intrusive and may not yield a satisfactory resolution to the situation. Although the evaluation of infertility proceeds, couples should be instructed to continue attempting pregnancy through intercourse timed to the most fertile days of the cycle. Less than 40% of couples with primary infertility conceive after 6 years of therapy compared with more than 50% of secondary infertility couples who conceive by 3 years.