Fever: Hypothalamic Response to Systemic Inflammation
 |
| CYTOKINES AND PROSTAGLANDINS CAUSE THE SICKNESS RESPONSE |
During systemic infections, there is a characteristic, hypothalamically mediated “sickness response” that includes an array of adaptive adjustments. Among these are a feeling of malaise, achiness, and sleepiness (which reinforces rest); increased secretion of adrenocortico-steroids (to mobilize adipose energy stores); and anorexia (to keep blood sugar low because many microorganisms prefer sugars as fuel, while the human body can adapt to using fat stores such as ketone bodies). However, the most prominent symptom of the “sickness response” is an elevation of body temperature called a fever. Experimental studies show that white blood cells are more active at 39° C than 37° C, while many microorganisms are less able to defend them-selves at this temperature.
There are
several processes by which invading infectious organisms can set off the
sickness response. One is that they can act locally on white blood cells that
then produce circulating hormones called cytokines. The cytokines can have
direct actions on certain types of neurons, but most of the “sickness response”
is due to the cytokines (or certain components of invading bacteria themselves)
inducing white blood cells and vascular endothelial cells to make
prostaglandins. The primary role of prostaglandins in the sickness responses is
demonstrated by the fact that inhibitors of cyclooxygenase, the enzyme that
produces prostaglandins, is sufficient to prevent most of these responses.
Prostaglandins
can act on receptors on peripheral nerves, but they also can cross the blood-brain
barrier and act directly on brain neurons that express prostaglandin receptors.
The prostaglandin that is probably most important for causing sickness
responses is prostaglandin E2 (PGE2), and it has a series of four different
E-type prostaglandin receptors (EP receptors) that are found on different
classes of cells in the central nervous system (CNS). For example, EP3
receptors in the median preoptic nucleus recognize PGE2 during an inflammatory
response and are critical for causing a fever response. Activation of
corticosteroid secretion during a sickness response requires EP3 receptors in
the preoptic area and the ventrolateral medulla, as well as EP1 receptors,
which may be in the paraventricular hypothalamic nucleus or the central nucleus
of the amygdala. Increased sensitivity to pain during fever is likely to be due
to EP3 receptors, but the exact locus of those receptors is not yet known.
The fever
response during sickness appears to be due to neurons in the median preoptic
nucleus with-drawing γ-aminobutyric acid
(GABA)ergic inhibition of the neurons in the paraventricular and dorsomedial hypothalamic
nuclei and the medullary raphe that produce elevated body temperature. This
allows body temperature to rise by about two to three degrees centigrade. Fever in the range
of 39° C to 40° C is uncomfortable but may be an adaptive response to help
fight off invading organisms.
Changes in
cognitive capacity and sleepiness during a sickness response are less well
understood. EP1 and EP3 receptors are found on hypothalamic preoptic neurons
that cause sleepiness, and EP4 receptors are found on histaminergic neurons in
the posterior hypothalamus, which may cause arousal. However, prostaglandins
are also made by the leptomeninges, and may have direct effects on cortical
neurons. PGE2 may also exacerbate meningeal and vascular pain perception
(causing headache, particularly during coughing or straining, which increase
intracranial pressure).
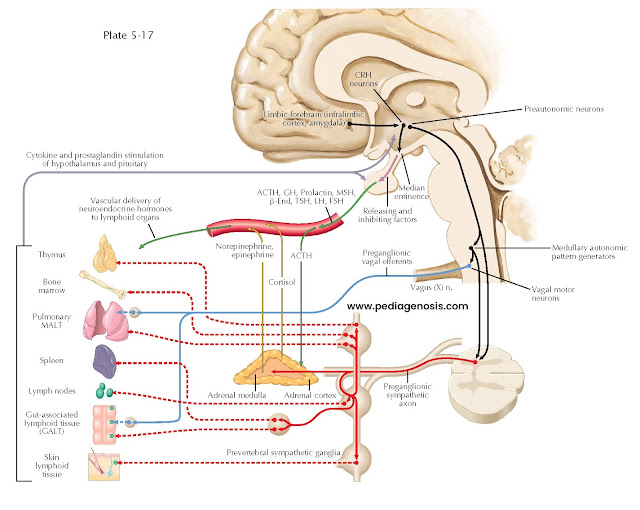
HYPOTHALAMIC RESPONSES DURING INFLAMMATION MODULATE IMMUNE RESPONSE
HYPOTHALAMIC
CONTROL OF LYMPHOID TISSUE IN IMMUNE RESPONSE
A critical part
of fighting off any infection is the activation of an appropriate immune
response. During a sickness response, prostaglandin E2 acts on neurons in the medulla,
amygdala, and hypothalamus, which results in an increase in the secretion of
corticotropin-releasing hormone (CRH) into the pituitary portal circulation,
elevated adrenocorticotropic hormone (ACTH) secretion by the pituitary gland,
and increased levels of circulating adrenal corticosteroids. Cortisol then
causes demargination of white blood cells that are adherent to the endothelium
of blood vessels, elevating the circulating white blood cell count. Lymphocytes
in a variety of tissues also respond directly to ACTH, and to a number of other
circulating hormones.
There is also direct sympathetic innervation of the lymphoid tissues. This input, which is also under hypothalamic control, may control the production and traf-ficking of specific lymphocyte subsets.


.webp)
_Page_049.jpg)
