Emergency Management and Assessment and Neurology Examination
 |
| FULL OUTLINE OF UNRESPONSIVENESS SCORE (FOUR) |
EMERGENCY MANAGEMENT AND ASSESSMENT
The many causes of coma are described elsewhere in this atlas (see Sections 9—Cerebrovascular Circulation and Stroke; 11—Infection of the Nervous System; 12—Neuro-Oncology; and 14—Head Trauma). Immediate care, regardless of the cause of diminished consciousness, must include attention to adequacy of spontaneous ventilation and blood pressure to maintain homeostasis. Thereafter, the emergency treatment of comatose patients follows accurate diagnosis that depends on history-taking, examination findings (including the evolution of neurologic symptoms and signs), and accompanying non-neurologic problems.
Coma
Scales. The Glasgow Coma Scale score (see Section 14, Plate 14-15) for best motor response in
either the upper or lower limbs is rated on a scale of 1 (no response) to 6
(patient-obeys commands). If there is no response or an incomplete reaction to
verbal stimuli, a noxious stimulus is applied, preferably to the medial side of
the arms or legs, to differentiate a localizing response from abnormal flexor
or extensor posturing. If the patient moves the limb toward (rather than away
from) the noxious stimulus, the response is not consistent with localization.
The patient’s reaction is classified as fending-off movements with localization
of pain (score 5), fending-off movements without localization of pain (4),
abnormal flexion (3), abnormal extension (2), and no response (1). A localizing
response indicates that the stimulus at more than one site causes a limb to
move so as to attempt to remove it. A flexor response in the upper limb
may vary from rapid withdrawal, associated with abduction of the shoulder, to a
slower decorticate posture, with adduction of the shoulder. An extensor
response is abnormal and usually associated with adduction, internal
rotation of the shoulder, and pronation of the forearm. No response is
usually associated with hypotonia. The Glasgow Coma Scale score alone is not an
adequate assessment of brainstem function. Further, it does not assess vital
signs (blood pressure, heart rate, body temperature, blood sugar), ability to
protect the airway and clear any airway obstruction (cough and gag), and
suggests what support or intervention is required to restore homeostasis. A
newer Full Outline of UnResponsiveness (FOUR)
scoring system measures impaired consciousness and specific brainstem
responses (see Plate 6-4). The four variables assessed are motor response,
brainstem reflexes, eye response, and respiratory pattern. The acronym
additionally reflects the number of categories and the maximum number of
potential points in each category.
After immediate
assessment, the next step is to initiate necessary emergency interventions for
life support. For example, an adequate airway must be assured, and an
intravenous line should be placed. If the patient is hypoventilating,
endotracheal intubation with assisted mechanical respiration should be
considered. Intravenous fluid bolus and vasopressors may be needed to treat
hypotension. Blood samples should be drawn for measurement of electrolytes, glucose,
toxicology, and arterial acid-base and blood gases. Serum is saved for further
study if necessary. When bedside testing shows the patient to be hypoglycemic,
an intravenous bolus of dextrose should be administered. If narcotic abuse is
suspected or if the patient does not respond to supportive measures, an
opiate-receptor antagonist, such as naloxone, can be given intravenously.
Next, after any
necessary immediate treatment is instituted, steps are taken to determine the
cause of coma with a robust and thorough history and appropriate
investigation. The patient’s family, friends, or physician can often supply
useful diagnostic information. Inquiries may elicit a history of diabetes;
previous renal, hepatic, or cardiac disease; severe depression; or drug use or
abuse. It is important to know what prescription medications have been used and
whether the patient had experienced any prodromal symptoms, such as headache,
unilateral weakness, and ataxia, or previous episodes of stupor.
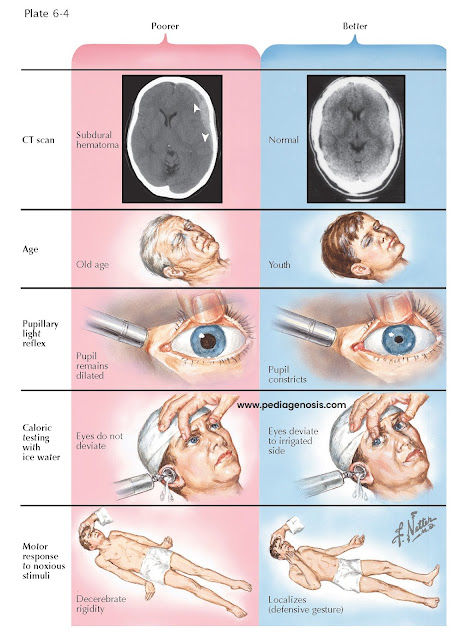 |
| PROGNOSIS IN COMA RELATED TO SEVERE HEAD INJURIES |
It is important
to carry out careful physical and neurologic examinations. Evaluation of the
patient’s spontaneous limb and bulbar movements, pupillary reactions, eye
movements, and response to painful stimuli usually indicates the level of brain
lesion causing coma. If the patient is able to blink, yawn, lick, and swallow,
which are complex brainstem reflexes, lower brainstem function is preserved.
Pupillary
size depends
on the balance between sympathetic function (descending sympathetic fibers course
in the lateral brainstem tegmentum) and parasympathetic function
(parasympathetic fibers exit with the oculomotor [cranial nerve III] in the
midbrain).
Pupillary reaction depends on the afferent light stimulus reaching the superior colliculus, as well as efferent transmission through the oculomotor nerve. The light reflex arc is located in the diencephalon and midbrain. Eye movements are observed by retracting the upper eyelids and watching spontaneous activity. When the head is rotated to one side—a maneuver to be performed only when it is clear that the cervical spine is not injured—the eyes should move fully and conjugately in the opposite direction if the appropriate brain-stem oculomotor and vestibular centers are preserved (doll’s eye phenomenon, or oculocephalogyric reflex). When the head is moved to the right, the eyes move conjugately to the left; when the head is moved down-ward, the eyes should roll upward. Ice water introduced into one ear canal with the patient’s head-of-bed elevated to 30 degrees should evoke conjugate eye movements toward the side of the stimulation (vestibulo-ocular reflex). In this position, the horizontal semicircular canal is in a vertical position, and the endolymph falls within the canal, thereby decreasing the rate of vestibular afferent firing. The eyes turn toward the ipsilateral ear, with horizontal nystagmus to the contralateral ear. Horizontal reflex eye movements are controlled by the oculomotor, trochlear (cranial nerve IV), and abducens (cranial nerve VI) nerves and their nuclei; the medial longitudinal fasciculus and parapontine reticular formation (pontine lateral gaze center); and the vestibular nuclei and nerves (cranial nerve VIII). All these structures are located within the pontine tegmentum. Vertical movements are controlled by centers in the rostral midbrain and caudal diencephalon.
Last, spontaneous limb movements should be observed. If absent, then testing for a response to a noxious stimulus is appropriate.


.webp)

