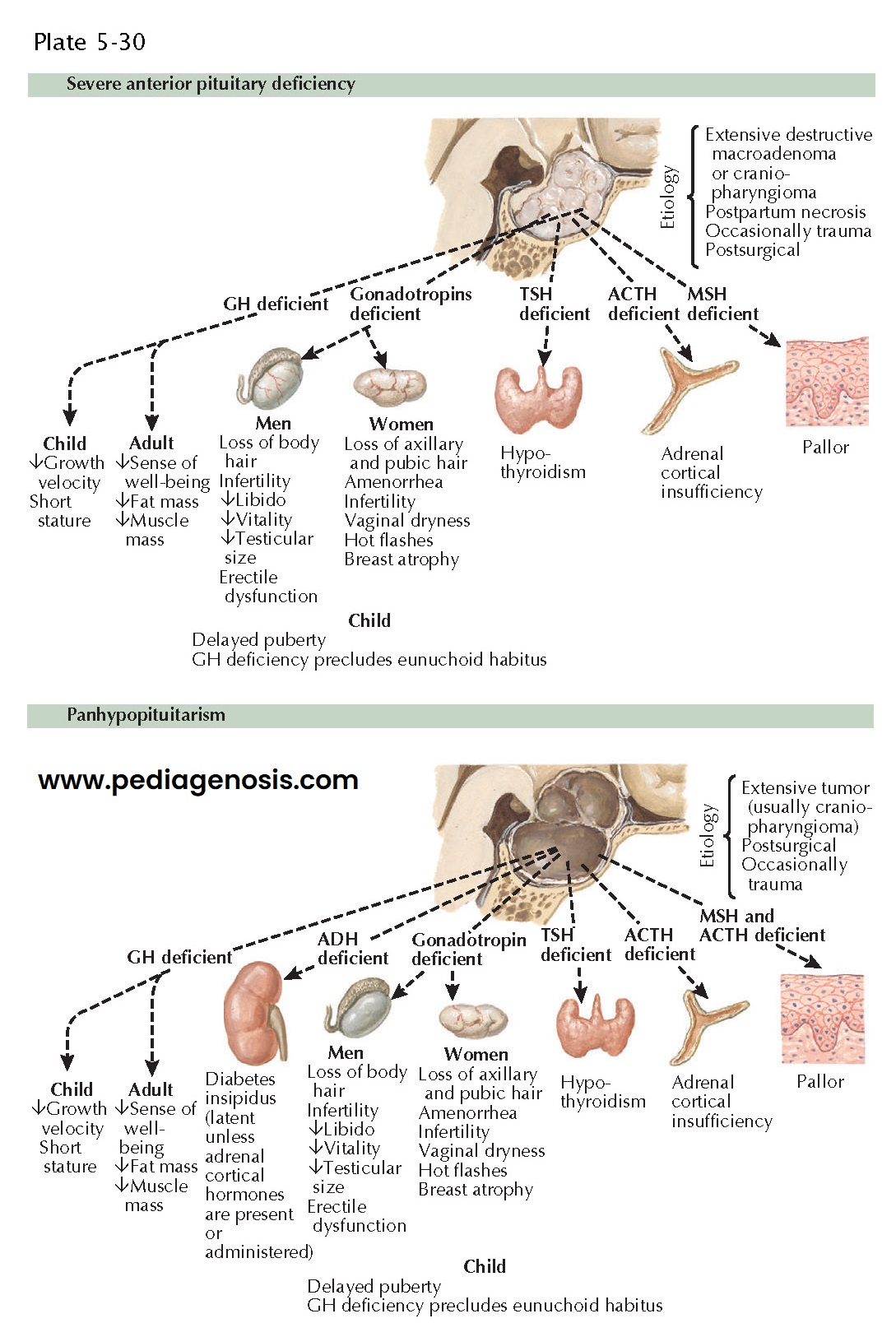
Severe Anterior Pituitary Hormone Deficiencies (Panhypopituitarism)
Extensive space-occupying
lesions within the sella or hypothalamus may lead to complete loss of anterior
pituitary function. Of note, the term panhypopituitarism is indicative
of complete loss of both anterior and posterior lobe function.
Pituitary macroadenomas, which, by definition, exceed 10 mm in greatest diameter, may cause multiple anterior pituitary hormone deficiencies but only rarely cause diabetes insipidus preoperatively. In contrast, large suprasellar tumors that impinge on the hypothalamus, stalk, and pituitary, including craniopharyngiomas, may disrupt both anterior and posterior lobe function. Similarly, pituitary surgery or trauma may lead to panhypopituitarism.
Gonadotropin
deficiency leads to lack of pubertal development, if it occurs before adolescence. Of
note, a eunuchoid habitus is unlikely to develop in young patients with
concurrent growth hormone deficiency. In adults of both genders, severe
gonadotropin deficiency leads to central hypogonadism. Severe gonadotropin
deficiency of long standing leads to gonadal atrophy, including decreased size
of the ovaries in women and testes in men. In addition, there is a decrease in
size of the uterus, vagina, and breasts in women, including thinning of the
endometrium and vaginal epithelial atrophy. In men, there is a decrease in size
of the penis and prostate.
Thyrotropin
deficiency leads to central hypothyroidism. The thyroid gland becomes atrophic,
including thinning of the follicular epithelium. Corticotropin deficiency leads
to central hypoadrenalism, involving loss of cortisol and adrenal
androgen secretion. Portions of the adrenal cortex, including the zona
fasciculata and the zona reticularis, become atrophic in these patients. In
contrast, the zona glomerulosa remains structurally intact, and aldosterone
secretion is unaffected. These patients may often exhibit pallor, occurring as
a result of anemia and decreased skin pigmentation resulting from lack of corticotropin
action on skin melanocytes. Growth hormone deficiency leads to a
decrease in growth velocity in children or adolescents, resulting in short
stature if untreated. Hypoglycemia may occur in childhood and appears to be a
consequence of growth hormone and glucocorticoid deficiency. Growth
hormone–deficient adults may exhibit low exercise capacity, abnormal body
composition (decrease in lean body mass and bone mass and increase in fat
mass), dyslipidemia, insulin resistance, increased cardiovascular risk, and
impaired quality of life. Prolactin deficiency leads to failure of lactation
in women and has no discernible effects in men.
Lack of
antidiuretic hormone secretion leads to central diabetes insipidus. The presence of diabetes
insipidus signifies extensive damage to the hypothalamus or stalk. Of note,
disruption of the pituitary stalk below the diaphragma sellae is less likely to
cause diabetes insipidus than injury to the stalk at the level of the median
eminence. In cases where the stalk is damaged distally, some antidiuretic
hormone–secreting axon terminals are spared and may secrete sufficient
antidiuretic hormone to prevent the development of central diabetes insipidus.
It may also be noted that central diabetes insipidus may be clinically latent
in patients with corticotropin deficiency because glucocorticoids have an
important role in increasing free water clearance in the kidneys. In these
patients, glucocorticoid replacement may precipitate the clinical onset of
central diabetes insipidus. Lack of oxytocin secretion leads to no discernible
symptoms or deficits in humans.
Once clinically
suspected, the presence of pituitary hormone deficiencies can be established
through hormone testing. Assays for systemic levels of target gland hormones
(morning cortisol, free thyroxine, and testosterone) are most helpful in the
diagnosis of hypopituitarism. In the case of some hormones, including growth
hormone and cortisol, stimulation testing is used to evaluate secretory
reserve. Water deprivation testing is used to diagnose central diabetes
insipidus.
Replacement therapies are available for all pituitary hormone deficiencies except prolactin and oxytocin. The respective target gland hormone is administered in patients with central hypoadrenalism (hydrocortisone or prednisone) and central hypothyroidism (levothyroxine). Sex steroid replacement (testosterone in men and estrogen-progestin in women) is generally advised, if not contraindicated. If fertility is of immediate interest, gonadotropin therapy is recommended in patients of both genders. Growth hormone replacement is advised in children, if not contraindicated. Although not essential for life, growth hormone replacement in adults is available in the United States and several other countries and may improve exercise capacity, body composition, several cardiovascular risk factors, and overall quality of life. Desmopressin, an analog of antidiuretic hormone that is devoid of vasopressor activity, is recom ended in patients with central diabetes insipidus.