TRACHEOSTOMY
Tracheostomy can be performed via an open surgical technique or via a percutaneous dilational technique. Percutaneous tracheostomy is becoming more popular because it is at least as safe as the surgical approach and is likely associated with fewer complications, primarily bleeding and infection. The choice between the two techniques typically depends on operator preference.
Key anatomic landmarks include the thyroid cartilage,
cricoid cartilage, cricothyroid membrane, first and second tracheal rings, and
sternal notch. The ideal insertion site for either technique is inferior to the
first or second tracheal ring. Tracheostomies placed in the cricothyroid
membrane have a higher incidence of tracheal stenosis, and those placed more
inferiorly than the third or fourth ring may have a higher incidence of
tracheoinnominate fistula formation.
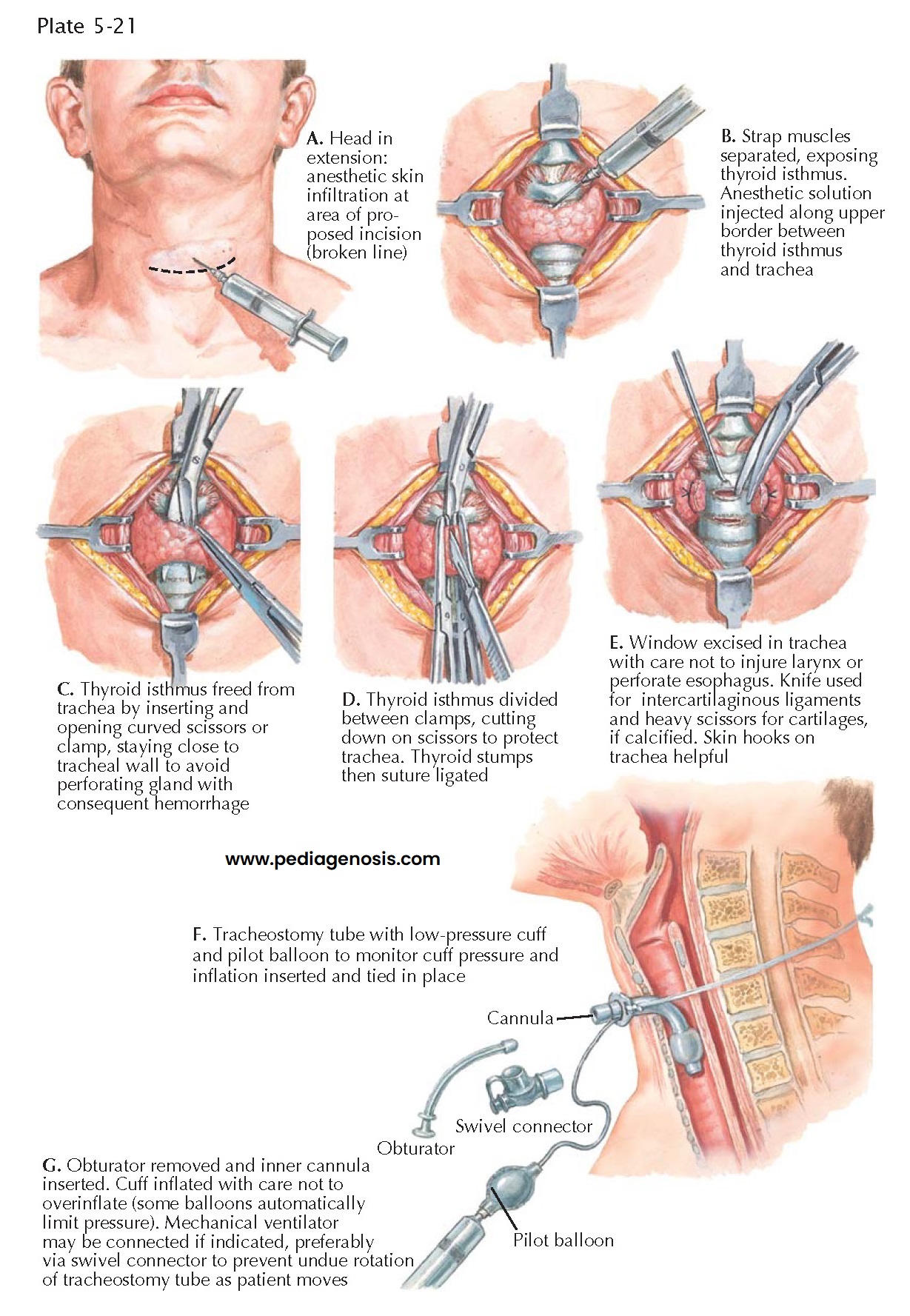
With a surgical tracheostomy, the strap muscles are
separated in the midline, exposing the isthmus of the thyroid gland. This
usually overlies the second and third tracheal cartilaginous rings. If not
retractable, the isthmus should be freed, divided, and ligated as illustrated.
A Björk flap, an inferiorly based inverted U-shaped flap, is then created and
sewn to the skin. A properly sized tracheostomy tube is then inserted and
securely fixed.
Percutaneous dilational tracheostomy uses the same
anatomic landmarks. After a small skin incision is made, blunt dissection is
performed to the level of the trachea. A guidewire is placed via the modified
Seldinger technique under bronchoscopic visualization, and the tract is
dilated, most commonly with a initial punch dilator and then a single tapered
dilator. The tracheostomy tube is then inserted and secured.
The classic silver-plated Jackson tracheostomy tubes
have been replaced over the past decade by a variety of nonirritating plastic
tubes. These have large-volume, low-pressure cuffs similar to endotracheal
tubes, allowing for mechanical ventilation with minimal
injury to the tracheal mucosa. Nonetheless, as with endotracheal tubes, cuff
pressures should be followed, and kept below 20 mm Hg.
Tracheostomy has several benefits over translaryngeal
intubation, including a requirement for less sedation, the ability to mobilize
patients without fear of losing an airway, and perhaps more rapid weaning from
mechanical ventilation and lower mortality rates.
One-way valves (Passy-Muir) offer the ability to speak
to some patients and can be of great psychological comfort to patients and
their families.
Damage to the trachea from tracheostomy tubes can occur at the top of the tube, at the stoma, or at the level of the inflatable cuff. Erosion may occur into the esophagus, particularly if prolonged use of a nasogastric tube is also necessary, or into a major vessel with usually fatal results.