INTRACAPSULAR FRACTURE OF FEMORAL
NECK
Femoral neck
fractures are very common injuries, especially in older persons. In young
persons, these injuries are usually caused by severe trauma. In older patients,
especially those with osteoporosis, they are associated with falls, and it is
possible that the fracture occurs before the fall.
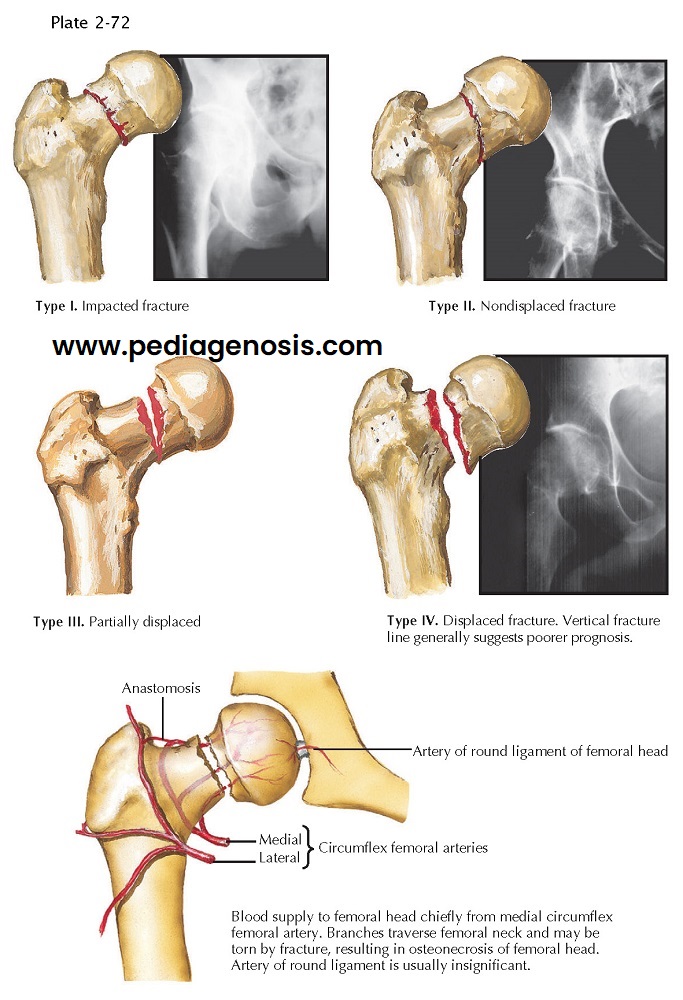
Garden has classified femoral neck fractures into four categories. In type I fracture, the superior portion of the femoral neck is impacted into the femoral head. Type II is a complete fracture that remains nondisplaced. Type III is a fracture with partial displacement between the femoral head and neck. In a type IV fracture, the femoral head is completely displaced from the femoral neck. The Garden classification is useful because it correlates the incidence of fracture nonunion and avascular necrosis of the femoral head with fracture displacement. The incidence of these complications is very low in type I injury, whereas the type IV fracture has a 33% risk of nonunion and a 30% risk of symptomatic avascular necrosis.
Management of femoral neck fractures involves reducing
the fracture in both the anteroposterior and lateral planes and achieving
secure internal fixation of the fracture fragments. Most fractures can be
reduced with closed means, using a variety of reduction techniques. In the
Leadbetter maneuver, reduction occurs with the hip in 90 degrees of flexion.
Other techniques involve reduction with the hip in extension or in only slight
flexion. Regardless of what method is used, near-anatomic reduction must be
achieved in both fracture planes; this is especially important in younger
patients. After reduction, the femoral neck fracture is securely fixated to
allow for impaction of the fracture fragments.
After surgery, the patient can begin gentle active and
passive range-of-motion exercises if the fixation is secure. Active
straight-leg raising is best avoided for the first 3 months. Patients who are
able to cooperate with a rehabilitation program are allowed gradual weight
bearing as healing of soft tissue and bone progresses. Patients who are not
able to cooperate are mobilized early from bed to chair, but weight bearing on
the injured limb is delayed.
Periodic follow-up is important to monitor fracture healing and to check for development of avascular necrosis of the femoral head. Initially, this tends to occur in the anterolateral segment of the femoral head, where damage to the vascular structures is greatest. If avascular necrosis is detected, intervention may be required to prevent the avascular segment from under-going late segmental collapse, which leads to degenerative changes in the hip joint.


.webp)

