PUERPERAL
INFECTION
Puerperal infection generally refers to an infection of the genital
tract in the postpartum period. For centuries, puerperal infection was the
leading cause of maternal death, though this has changed dramatically with the
advent of antibiotics. Maternal death rates associated with infection account
for approximately 0.6 maternal deaths per 100,000 live births. Endometritis is
the most common form of postpartum infection, though other sources of
postpartum infections include postsurgical wound infections, perineal
cellulitis, mastitis, respiratory complications from anesthesia or under-lying
pulmonary disease such as asthma or obstructive lung disease, retained products
of conception, urinary tract infections, and septic pelvic phlebitis. Overall,
postpartum infection is estimated to affect 1% to 3% of normal vaginal
deliveries, 5% to 15% of scheduled caesarean deliveries, and 15% to 20% of
unscheduled caesarean deliveries.
The organisms responsible for the vast majority of puerperal infections are the anaerobic and aerobic nonhemolytic varieties of streptococci. These organisms are usually present in the birth canal, becoming pathogenic when carried to the uterine cavity during or after delivery.
Postpartum endometritis
is typically a polymicrobial infection (70% of cases) involving a mixture of
two to three aerobes and anaerobes from the genital tract. In most cases of
endometritis, the bacteria responsible are those that normally reside in the
bowel, vagina, perineum, and cervix. Commonly isolated organisms include Ureaplasma
urealyticum, Peptostreptococcus, Gard- nerella vaginalis, Bacteroides
bivius, and group B streptococci. Other, though less frequent, organisms
causing puerperal infection are Staphylococcus albus (Micrococcus
pyogenes), anaerobic organisms, and the colon bacillus (Escherichia coli).
Chlamydia has also been associated with late-onset postpartum
endometritis.
Inadequate asepsis during
labor and delivery, repeated vaginal examinations, and the use of contaminated
materials are avoidable factors in the pathogenesis. Coitus late in pregnancy
also has been considered to help disseminate inoculation and infection. Blood
loss and trauma are considered the most frequent predisposing causes of
puerperal infection. Trauma creates a portal of entry and produces a favorable
environment for the development of virulent bacteria. Prolonged labor, particularly
with early rupture of the membranes, retention of placental tissues and major
vaginal procedures producing vaginal and cervical lacerations may initiate or
foster puerperal infection.
The pathologic findings in
puerperal infection are similar to those of any other wound infection.
Following delivery of the fetus and placenta, the endometrium favors bacterial
growth. Infection of the episiotomy and vaginal lacerations may occur, but
these are less frequent than endometritis. This latter is by far the most
frequent site of puerperal sepsis. The appearance of the endometrium and its
discharge vary according to the infecting organisms. It usually appears
necrotic and yellowish green but may be black from decomposed blood. The
inflammatory process may remain in the uterine cavity, spread to the parametrial
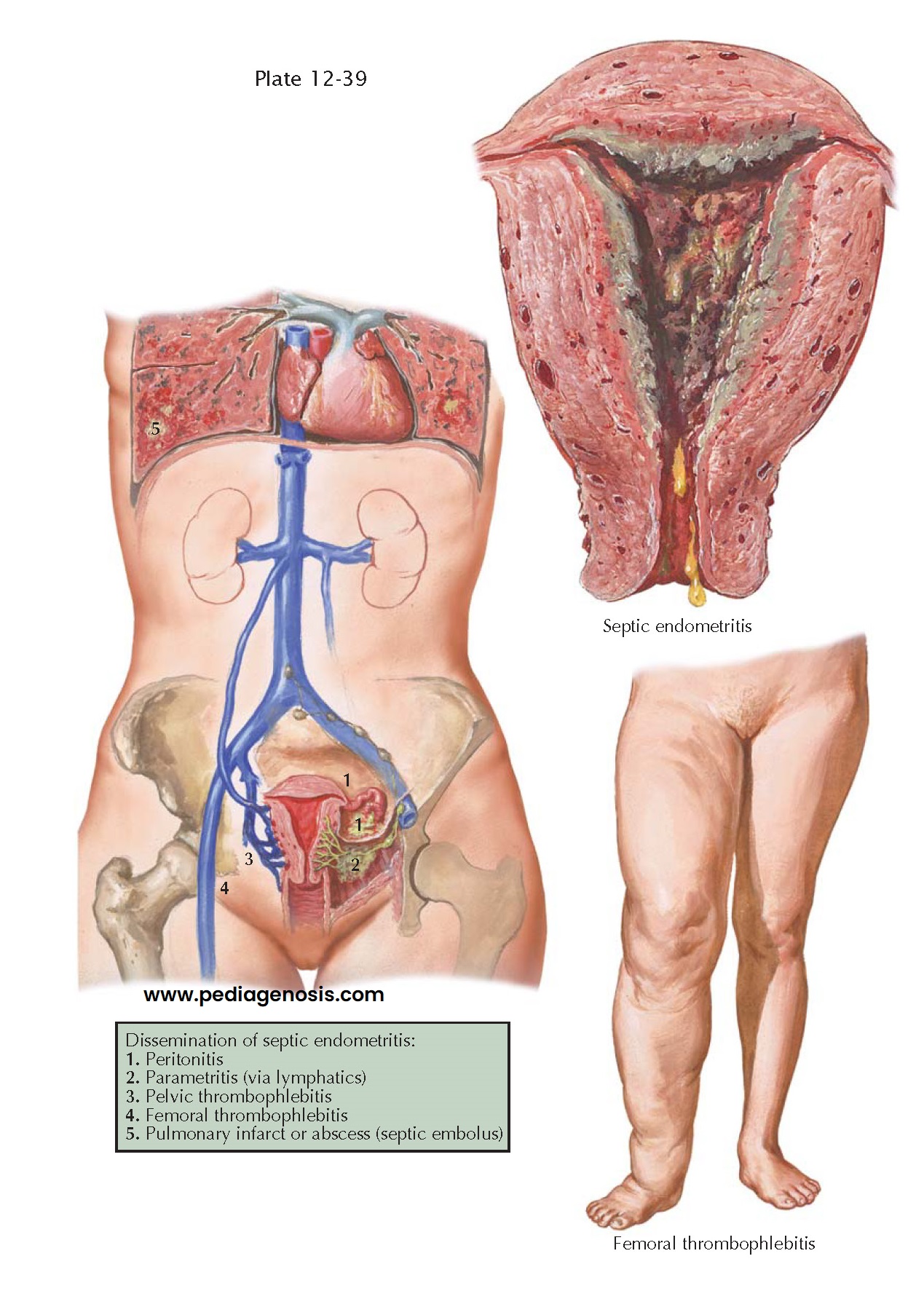
tissues, or become widely disseminated. From the endometrium, the inflammatory
process may extend along the uterine and other pelvic veins, resulting in
pelvic thrombophlebitis. Thrombophlebitis of the leg veins may also be seen. Extension of the inflammation
through the lymphatic channels to the parametrial tissues and peritoneum
results in parametritis, pelvic cellulitis, and peritonitis. Distant spread to
lungs or liver may occur in the form of septic emboli and therewith cause
septic infarcts and abscesses.
The diagnosis is usually made without difficulty. Fever occurring in the postpartum period, accompanied by lower abdominal tenderness, should be considered to be a puerperal infection until proved otherwise. Extreme abdominal and uterine tenderness together with rigidity of the abdominal walls and absence of peristalsis are indicative of generalized peritonitis. The character and odor of the lochia may help in making the diagnosis and sometimes in recognizing the organisms. Some infections, notably those caused by group A-hemolytic streptococci, may be associated with scanty, odorless lochia.