INFERTILITY III—EVALUATION OF MALE
Among infertile couples,
50% have causal or associated male factors. In addition, 2% of male factor infertility
is a result of an underlying, often treatable but possibly life-threatening medical
condition. For these reasons, the male evaluation is conducted systematically along
with the female assessment. The evaluation includes a history, physical examination,
semen analysis, and hormone assessment. Treatments include nonsurgical,
surgical, and assisted reproductive options.
The history reviews past and current attempts at paternity. Important medical problems to elucidate include fevers and systemic illnesses such as diabetes, cystic fibrosis, cancer, and infections. Prior surgery, including orchidopexy and herniorrhaphy; trauma; and retroperitoneal, pelvic, bladder, or prostate procedures may impair infertility. A family history of cryptorchidism, midline defects, or hypogonadism is also important. A developmental history of hypospadias, congenital anomalies, and medication use may be revealing. A social history may elucidate the habitual use of the gonadotoxins such as alcohol, tobacco, recreational drugs, and anabolic steroids. Spermicidal lubricants and incorrect patterns of timing intercourse may be noted from a sexual history. Lastly, an occupational history determines exposure to ionizing radiation, chronic heat, benzene-based solvents, dyes, pesticides, herbicides, and heavy minerals.
The physical examination assesses body habitus, including obesity, gynecomastia,
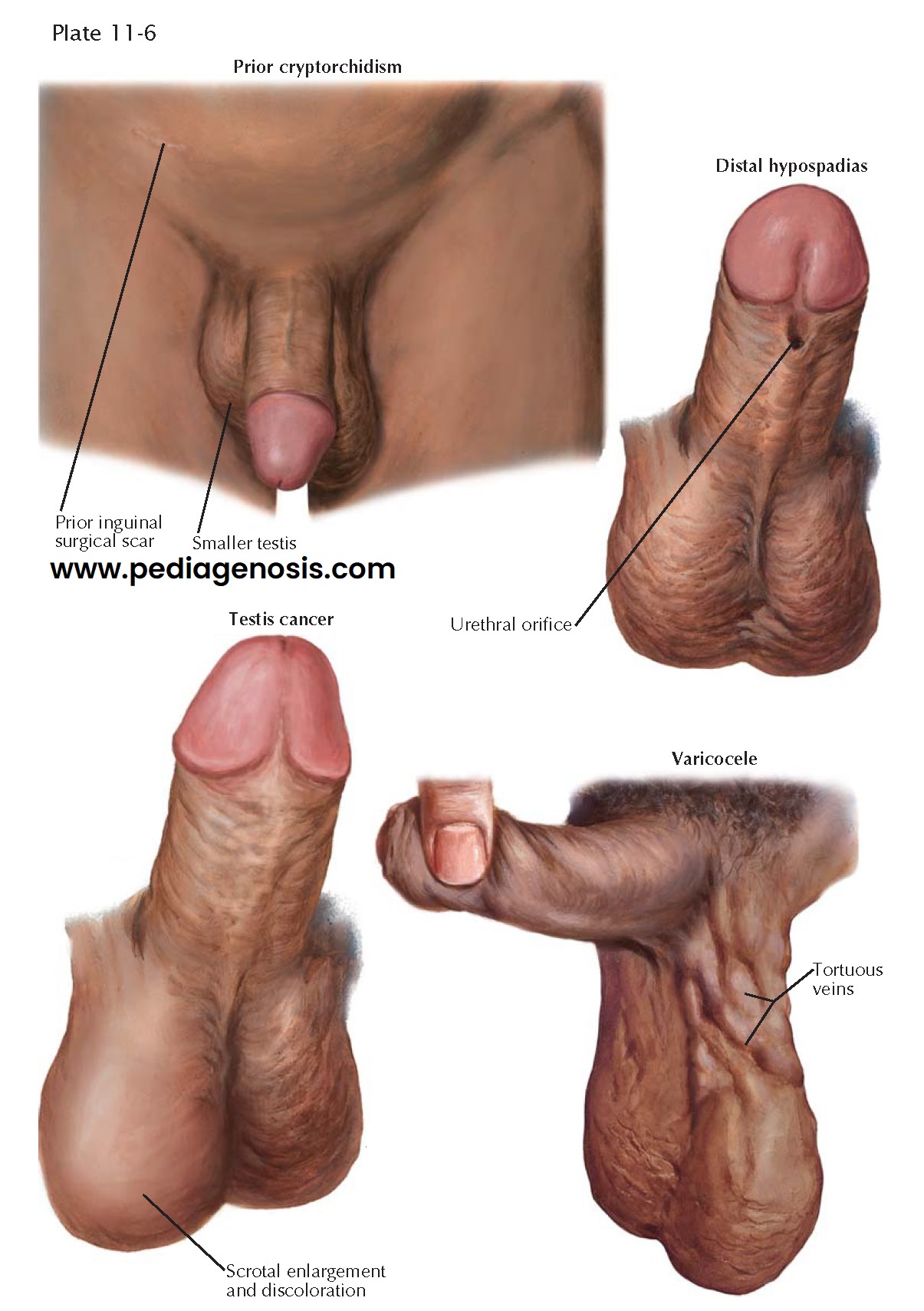
and secondary sex characteristics. The phallus may reveal hypospadias, chordee,
plaques, or venereal lesions. The testes should be evaluated for size, consistency,
and contour irregularities suggestive of a mass. Recall that 80% of testis
volume is determined by spermatogenesis; hence, testis atrophy is likely associated
with decreased sperm production. Palpation of the epididymides might reveal
induration, fullness, or nodules indicative of infections or obstruction. Careful
delineation of each vas deferens may reveal agenesis, atresia, or injury. The spermatic
cords should be examined for asymmetry suggestive of a lipoma or varicocele, lesions
differentiated by an examination in both the standing and supine positions.
Meaningful varicoceles are diagnosed exclusively by physical examination. Lastly,
a rectal examination is important in identifying large cysts or dilated seminal
vesicles, which can be associated with infertility.
Although not a true measure of fertility, the semen analysis, if abnormal,
suggests that the probability of achieving fertility is lower than normal. Two semen
analyses, performed with 2 to 3 days of sexual abstinence, are sought because of
the large biologic variability in semen quality. Lubricants should be avoided
and the specimen kept at body temperature during transport. Normal values have been
described, as out-lined in Plate 5-2. However, there is debate concerning
precisely what values are considered “normal.” Recall that spermatogenesis takes
70 to 80 days to complete, so that an individual semen analysis reflects biologic
influences occurring 2 to 3 months prior.
If the sperm concentration is low or there are signs of an endocrinopathy,
then a hormonal evaluation should also be performed. This should include an
assessment of the pituitary–gonadal axis with testosterone and follicle-stimulating
hormone levels. The chance of a clinically significant endocrinopathy presenting as infertility is approximately 2%.
The initial male evaluation may be normal or abnormal. If normal, further
consideration should be given to female factor evaluation, including a more thorough
assessment of ovulation, pelvic anatomy, and age-related fertility issues. If the
initial male assessment reveals abnormalities, then further male evaluation or treatment
is indicated. Adjunctive testing is undertaken depending on the findings but may
include transrectal or scrotal ultrasound to evaluation ejaculatory duct obstruction
or varicocele, semen testing for antisperm antibodies or leukocytes (see Plate 5-2),
postejaculate urinalysis, urine or semen cultures, semen fructose, or genetic testing
(see Plate 5-3). Correctable abnormalities in the male should be treated before
couples consider assisted reproduction.
Infertile couples with unremarkable female and male evaluations are termed unexplained infertility. In such cases, further evaluation of male factor infertility is warranted, yet a precise algorithm to follow has not been defined. Antisperm antibodies and poor chromatin structure, the latter reflective of increased levels of denatured sperm DNA, can each be found in 10% of semen analyses in such cases. Tests of sperm function such as the sperm penetration assay or the hemizona assay may also be considered. Finally, many couples proceed to assisted reproduction with intrauterine insemination.


.webp)
_Page_049.jpg)
